Adipose tissue is more than stored fat. It is an active endocrine organ that releases hormones, cytokines, and signaling molecules that influence appetite, insulin sensitivity, inflammation, and organ function throughout the body. Adipose-derived stem cells sit at the center of this system, and in obesity and metabolic disease they can act in ways that either worsen or, in some experimental contexts, potentially help correct metabolic dysfunction. Understanding which is which, and under what conditions, is where the current research stands.
TLDR: Adipose-derived stem cells change their behavior substantially in obesity and type 2 diabetes. In some experimental models, they contribute to inflammation and insulin resistance through altered secretion and extracellular vesicle signaling. In other models, their secreted factors and extracellular vesicles improve insulin sensitivity and reduce fatty liver disease markers. A small number of human studies have explored SVF or ADSC infusions in diabetes and liver disease, but these approaches remain investigational and are not a replacement for established treatments.
Important Disclaimer: Save My Fat does not provide diabetes, obesity, or fatty liver disease treatment and does not offer systemic stem cell therapies of any kind. No adipose-derived stem cell or SVF therapy is FDA-approved to treat or cure type 2 diabetes, obesity, NAFLD, or NASH. This article summarizes published research for educational purposes only and does not constitute medical or legal advice. Patients must discuss all treatment and research decisions with their endocrinologist, primary care physician, or hepatologist.
Someone living with type 2 diabetes for years, or with a recent diagnosis of non-alcoholic fatty liver disease, may come across a clinic advertising “fat stem cell infusions to reset your metabolism” and wonder whether this is a breakthrough their doctor has not mentioned. That experience is increasingly common, and it reflects a real underlying tension in the science: adipose-derived cells do influence metabolism in meaningful ways in laboratory and animal research, and the gap between that science and a proven clinical therapy is substantial.
The biological connection between adipose tissue and metabolic disease is not speculative. It is among the most studied relationships in endocrinology and cell biology. What remains uncertain is whether the experimental signals from preclinical models will translate into safe, effective therapies in humans, and the path from “interesting mouse model results” to “standard clinical care” is long, regulated, and expensive.
This guide explains how adipose tissue functions as an endocrine organ, how the stem cells within it change in the setting of obesity and diabetes, what the current preclinical and early human data show for diabetes and fatty liver disease, and what all of that does and does not mean for tissue banking.
Adipose Tissue as an Endocrine Organ
Beyond “Storage”: Adipokines and Inflammation
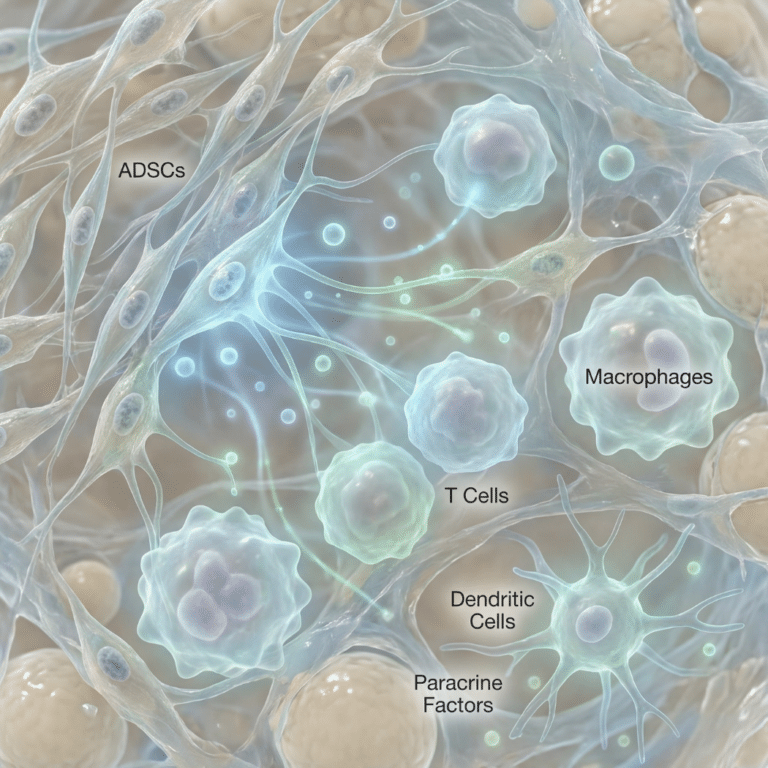
Adipose tissue is composed of more than fat-storing adipocytes. It contains a stromal vascular fraction (SVF) that includes adipose-derived stem cells (ADSCs), endothelial cells, immune cells including macrophages, pericytes, and blood vessels. This heterogeneous tissue functions as a genuine endocrine organ, releasing hormones and cytokines called adipokines that circulate to distant tissues and influence whole-body physiology.
Key adipokines include leptin, which signals satiety and energy balance to the brain, and adiponectin, which improves insulin sensitivity and has anti-inflammatory properties. In obesity and metabolic disease, adipokine profiles shift: leptin resistance develops, adiponectin levels fall, and pro-inflammatory cytokines including tumor necrosis factor-alpha (TNF-alpha) and interleukin-6 (IL-6) rise. This inflammatory shift affects how other tissues, including liver, muscle, and pancreatic beta cells, respond to insulin.
What Changes in Obesity
As adipose tissue expands in obesity, its cellular environment changes in ways that affect the resident ADSCs. Reviews in the metabolic ADSC literature, including the “spear and shield” analysis at PMC10066342 and the 2025 Frontiers in Endocrinology review at frontiersin.org, describe how obesity is associated with increased macrophage infiltration into adipose tissue, formation of inflammatory crown-like structures around dying adipocytes, and chronic low-grade tissue inflammation. In this environment, ADSC proliferation slows, differentiation capacity declines, and secretory profiles shift toward more pro-inflammatory patterns.
These changes matter because ADSCs in obese adipose tissue do not behave like ADSCs in lean, healthy tissue. The cells retain their identity but operate differently, a distinction that carries direct implications for both understanding how metabolic disease progresses and for interpreting what autologous cell therapies from obese donors might actually deliver.
Where ADSCs Fit in This System
ADSCs perform several roles in adipose tissue homeostasis. They generate new adipocytes as needed, maintaining adipose tissue turnover and function. They secrete paracrine factors that support the local vascular network, regulate immune cell behavior, and communicate with mature adipocytes. In a metabolically healthy state, these functions support tissue integrity. In a chronically inflamed, obese state, the same cells may amplify dysfunction rather than correct it, depending on which signals they are receiving and sending. For a foundation on what ADSCs are and how they are characterized, the patient’s guide to adipose-derived stem cells covers the basic biology.
The “Spear and Shield” Concept for ADSCs in Obesity
The “spear and shield” framing is used in the published literature to capture a genuine duality in how adipose-derived cells interact with metabolic disease. The same cell type that in some contexts appears to drive metabolic dysfunction can in other contexts produce factors that counteract it.
ADSCs as a “Spear” in Metabolic Disease
In the setting of obesity and insulin resistance, ADSCs and the extracellular vesicles (EVs) they release can contribute to metabolic dysfunction through several mechanisms described in the PMC10066342 review and the review of obesity and adipose-derived EVs at PMC11853251. Obesity-conditioned ADSCs show altered cytokine secretion that can promote macrophage polarization toward pro-inflammatory states in adipose tissue, amplifying the chronic inflammation that drives insulin resistance.
At the EV level, specific microRNAs (miR-27a, miR-222, and others) carried by adipose-derived vesicles from obese donors have been linked in preclinical models to impaired insulin signaling in skeletal muscle and liver, the key tissues where insulin resistance manifests clinically. These microRNAs can suppress components of the insulin signaling cascade in recipient cells, providing a mechanism by which adipose tissue communicates its dysfunctional state to distant organs.
ADSCs as a “Shield” in Experimental Models
The same cell type, when derived from lean donors or specifically prepared for therapeutic use, can produce a different set of signals. In experimental models described in the spear and shield review and related literature, ADSCs and their EVs have demonstrated anti-inflammatory effects, reductions in liver fat accumulation (hepatic steatosis), and improvements in insulin sensitivity in obese and diabetic mouse models. Specific EV preparations have been reported to improve beta-cell adaptation and glucose tolerance in insulin-resistant models by delivering a different cargo of microRNAs and proteins that support insulin pathway function.
Why Both Can Be True
The apparent contradiction resolves when the context is held in view. The same cell type produces different secretory outputs depending on the donor’s metabolic state, the local inflammatory environment, the preparation method (fresh vs. cultured vs. EV-isolated), the target tissue, and the model system being studied. Obesity-derived ADSCs produce a different functional profile from lean-derived ADSCs. The same donor’s cells behave differently when placed in an inflamed versus a metabolically healthy tissue environment.
This is not a failure of the science. It accurately reflects the biology of a cell type that is highly responsive to its environment. It also means that extrapolating any single finding, whether apparently harmful or beneficial, to broad clinical recommendations is scientifically premature.
ADSCs and Stromal Vascular Fraction in Type 2 Diabetes Research
Mechanisms in Preclinical Diabetes Models
The 2023 review in the Journal of Clinical Endocrinology and Metabolism on adipose-derived MSC therapy as a new option for diabetes, available at academic.oup.com, describes the primary mechanisms under investigation in preclinical models. In rodent models of type 2 diabetes and insulin resistance, AD-MSCs have been shown to improve insulin sensitivity through multiple pathways: enhancing insulin receptor signaling and Akt phosphorylation (a key step in insulin’s intracellular cascade) in muscle and adipose tissue, increasing expression and membrane translocation of GLUT4 (the glucose transporter that moves glucose into cells in response to insulin), and modulating pro-inflammatory cytokines including TNF-alpha and IL-6 in a direction that reduces insulin antagonism. Some studies describe support for pancreatic beta cells through ADSC-secreted growth factors.
These mechanisms are biologically coherent and align with what is known about the pathophysiology of type 2 diabetes. They form a scientific rationale for continued clinical investigation. They do not, by themselves, prove that human patients would experience comparable effects.
Early Human Studies of SVF or ADSCs in T2D
A small number of human studies have examined cell-based approaches in type 2 diabetes. NCT01453751 was registered to evaluate safety and exploratory metabolic endpoints of intravenous autologous adipose-derived stromal cell infusion in type 2 diabetes patients, with primary outcomes including safety monitoring and exploratory measurements of HbA1c and insulin requirements.
A small uncontrolled clinical series published in Clinical Diabetology, available at journals.viamedica.pl, studied the combination of autologous SVF with platelet-rich plasma (PRP) in a group of type 2 diabetes patients. The series reported statistically significant short-term reductions in HbA1c, a standard measure of average blood glucose control, in the treated group. The authors noted important limitations: the series was uncontrolled, meaning there was no comparison group receiving standard care alone; the number of patients available at the 12-month follow-up was very small; and the contribution of the SVF versus the PRP versus general clinical attention could not be separated. These results are reported here exactly as the study described them, with their limitations intact.
What These Studies Do and Do Not Show
Human studies of ADSCs and SVF in type 2 diabetes to date have generated signals that researchers consider worth pursuing but have not established safety or efficacy for general clinical use. They are uniformly small, frequently open-label or uncontrolled, and have short follow-up relative to the lifelong nature of type 2 diabetes. A study showing that HbA1c decreased over three to six months in an uncontrolled setting does not demonstrate that the decrease would persist, that the cell infusion caused the decrease rather than concomitant lifestyle or medication changes, or that the procedure is free of rare adverse events that a small study cannot detect.
ADSCs and Fatty Liver Disease (NAFLD and NASH)
Why Fatty Liver Is a Research Target
Non-alcoholic fatty liver disease (NAFLD) is defined by excess fat accumulation in the liver not explained by alcohol use. Non-alcoholic steatohepatitis (NASH) is the more severe inflammatory form, characterized by liver cell injury and fibrosis in addition to fat. Both conditions are strongly associated with obesity and insulin resistance, and NASH can progress to cirrhosis and liver failure. Established treatments focus on weight loss, glycemic control, and management of metabolic risk factors. No cell therapy is approved as standard care for NAFLD or NASH, and there is a recognized unmet need for treatments that address the underlying liver injury in patients who do not achieve adequate improvement with lifestyle and medications alone.
Preclinical Data with ADSCs and EVs in NAFLD and NASH
Research reviewed at PMC9481107, examining ADSC-secreted EVs in NAFLD, and a study at PMC10728850 examining the effects of LPS-stimulated ADSCs in NAFLD models, describe preclinical findings including improved liver histology, reduced inflammatory gene expression, restoration of autophagic flux (a cellular quality-control process that is impaired in NASH), and reduced markers of endoplasmic reticulum stress in high-fat diet-induced NASH mouse models. ADSC-derived exosomes carrying specific microRNA cargo have been shown in NAFLD models to reduce liver lipid accumulation and fibrosis by modulating transcription factors involved in lipid metabolism.
These are animal and cell culture findings. They establish mechanistic plausibility and support continued investigation, but do not demonstrate that human NAFLD or NASH patients would experience comparable benefits.
Translation to Humans
As of April 2026, human clinical trials of ADSCs or their EVs in NAFLD or NASH are at very early stages. Published human evidence is limited to isolated case reports and very small pilot series. No phase II or III trial results are available demonstrating safety and efficacy of any ADSC-based intervention in human NAFLD or NASH. The field is moving from preclinical mechanistic work toward early-phase human studies, but this transition takes years to complete responsibly.
Adipose-Derived Extracellular Vesicles in Metabolic Research
EVs as Metabolic Messengers
Extracellular vesicles (EVs, the broad category that includes exosomes and microvesicles) are small membrane-bound particles that cells release carrying proteins, lipids, and RNA molecules including microRNAs. The PMC11853251 review of adipose-derived EVs in obesity and metabolic disease describes how adipose tissue releases large quantities of EVs that circulate to liver, muscle, and other metabolically active tissues. These vesicles carry cargo that can alter gene expression and cell behavior in recipient tissues without delivering whole cells.
In the context of obesity, some adipose-derived EVs carry microRNAs that inhibit key components of the insulin signaling cascade in muscle and liver, providing a paracrine mechanism for how expanded, inflamed adipose tissue communicates metabolic dysfunction to distant organs. This is active biology, not theoretical, and it has been demonstrated in multiple preclinical systems.
ADSC-Derived EVs as Potential Therapeutic Tools
In a therapeutic direction, EVs derived from lean or specially conditioned ADSCs have shown different cargo profiles with potentially beneficial effects. Specific studies in obese mouse models have reported improvements in insulin sensitivity and reductions in hepatic steatosis following ADSC EV administration, with some reports quantifying improvements in insulin sensitivity measurements in the range of 20 to 30 percent in the treated animals compared with untreated controls. EV preparations targeting specific microRNA pathways, such as miR-223-3p modulation, have reduced liver fibrosis markers in NAFLD models by influencing transcription factors involved in lipid and inflammatory signaling.
These are animal model findings and the numbers reported come from those specific experimental systems. They establish that the direction of effect is biologically coherent and that the magnitude of effects in those models is potentially meaningful. Whether similar effects would occur in human patients, at what doses, by what delivery route, and with what safety profile, remains to be established.
Status of EV-Based Metabolic Approaches
No ADSC-derived EV product is FDA-approved for any metabolic indication in the United States. Manufacturing consistency, optimal dosing, delivery route, and long-term safety have not been established for any ADSC EV metabolic application. This is an area of genuine scientific progress, but it remains firmly in the preclinical and very early translational phase.
How ADSCs Themselves Change in Obesity and Diabetes
Functional Decline in Obesity
The functional properties of ADSCs are not static across different donors or metabolic states. Reviews of ADSC biology in obesity consistently describe a pattern of reduced proliferation, impaired adipogenic and osteogenic differentiation capacity, and altered secretory output in cells from obese donors compared with lean donors. The immunomodulatory capacity that makes ADSCs scientifically interesting for regenerative and inflammatory applications may be diminished in obesity-derived cells.
This functional decline has practical implications. If future metabolic therapies rely on autologous ADSCs derived from the same patient being treated, the quality of those cells depends on the donor’s metabolic state. A person with severe obesity and type 2 diabetes may have a different cell quality profile than a metabolically healthy donor.
Diabetes and SVF Quality
Some studies examining SVF from diabetic patients have reported lower cell viability and altered cellular composition compared with non-diabetic donors. The SVF/PRP study in type 2 diabetes noted that SVF from diabetic patients may carry lower baseline cell viability, which the authors flagged as a variable that could influence both safety monitoring and any exploratory efficacy signal. This is not a settled question and remains an active area of research, particularly as the field considers how to screen and qualify autologous cell preparations for therapeutic use.
Why Donor Health Matters for Future Applications
If ADSC-based metabolic therapies eventually reach clinical approval, donor screening and cell quality criteria will need to account for metabolic status. Banking tissue from a person with severe metabolic disease may preserve cells with a different functional profile than banking from a younger, metabolically healthy person. Whether that difference would matter for any specific future application depends on what that application requires, which is not yet defined. This is a research question, not a clinical protocol.
What This Means for Patients and Tissue Banking
Banking Is Not a Metabolic Treatment
Banking adipose tissue through Save My Fat stores intact tissue in cryogenic preservation. It does not lower blood sugar, reduce liver fat, improve insulin sensitivity, or reverse metabolic syndrome. The complete guide to adipose tissue banking and the how banking works article explain in detail what the banking process involves and what it preserves. Any future metabolic use of banked tissue would require its own regulatory pathway, clinical trial evidence, and individualized medical decision-making that does not yet exist.
Present Realities vs Future Possibilities
The metabolic disease burden in the United States is enormous, and the inadequacy of current treatments for some patients creates real demand for alternatives. ADSC-based metabolic research is active, scientifically grounded, and may eventually produce clinically useful therapies. As of April 2026, none are standard care, and none are available outside of registered clinical protocols. The most effective proven interventions for metabolic disease remain dietary and lifestyle modification, evidence-based pharmacotherapy, and bariatric surgery where clinically appropriate.
These are not statements against research. They are an accurate description of where the science stands. For patients interested in clinical trial options, the guide to clinical trials for regenerative medicine explains how to evaluate registered trials and what enrollment actually involves. The emerging research page tracks areas of active investigation in the ADSC field.
How to Evaluate Metabolic Stem Cell Marketing Claims
Three straightforward questions reveal whether a clinic’s metabolic stem cell offering is grounded in responsible research. First, can they provide a ClinicalTrials.gov registration number (NCT number) for the specific protocol being offered? Second, is an IND in place from the FDA? Third, do they clearly describe the procedure as experimental and discuss alternatives including standard metabolic care? A clinic that cannot answer all three specifically is not operating within a registered, regulated research framework.
Frequently Asked Questions
Can adipose-derived stem cells cure type 2 diabetes today?
No. No adipose-derived stem cell or SVF therapy is FDA-approved to treat type 2 diabetes in the United States. Small, early-phase human studies have explored whether cell-based approaches can influence metabolic markers such as HbA1c in short-term, uncontrolled settings, and some have reported preliminary signals. These are not definitive evidence of efficacy, and they do not establish safety for broad clinical use. Type 2 diabetes management must remain grounded in evidence-based care including medications and lifestyle interventions under physician supervision.
What have small human studies of SVF or ADSC infusions in diabetes actually shown?
The published human studies in this area are small, open-label series and registered pilot trials. A study combining autologous SVF with platelet-rich plasma in type 2 diabetes patients reported short-term HbA1c reductions in treated patients. A registered intravenous SVF safety trial (NCT01453751) evaluated tolerability and exploratory metabolic endpoints. These studies show that cell-based approaches can be administered without major acute adverse events in small, carefully monitored groups, and that some metabolic markers changed in treated patients. They do not establish that ADSCs or SVF are safe and effective for type 2 diabetes in a broader population.
How are ADSCs being studied in fatty liver disease (NAFLD and NASH)?
Most ADSC and EV research in NAFLD and NASH is currently preclinical, conducted in cell culture systems and animal models including high-fat diet-induced NASH in mice. Studies described in PMC9481107 and PMC10728850 document reduced liver inflammation, improved autophagy, and lower fibrosis markers in treated animals. Human trials in NAFLD and NASH using ADSC-based approaches are at early stages. No therapy has reached phase III or received FDA consideration for any of these indications.
Do fat stem cells from obese people behave differently from those in lean people?
Yes, according to multiple published reviews. ADSCs from obese donors consistently show reduced proliferation, impaired differentiation, altered cytokine secretion, and in some studies reduced immunomodulatory capacity compared with cells from lean donors. This is one reason that the “spear and shield” concept reviewed at PMC10066342 is scientifically meaningful: donor metabolic status is a significant variable in how these cells behave. Whether this difference would affect any specific future therapeutic application depends on what that application requires, and that level of specificity does not yet exist.
What are adipose-derived extracellular vesicles and how do they affect insulin resistance in research?
Extracellular vesicles (EVs) are small membrane-bound particles released by cells that carry biological cargo including microRNAs, proteins, and lipids to recipient cells. Adipose-derived EVs from obese donors carry microRNAs that can impair insulin signaling in muscle and liver in preclinical systems, contributing to insulin resistance. EVs derived from lean or therapeutically conditioned ADSCs carry different cargo and have shown improvements in insulin sensitivity and hepatic fat in animal models, as reviewed at PMC11853251. All of these are preclinical findings; no adipose-derived EV product is approved for human metabolic disease.
If I bank my fat now, does that mean I can use it later to fix my metabolism?
No. Banking preserves your tissue in cryogenic storage. It does not provide any metabolic benefit today and does not guarantee access to any future metabolic therapy. If ADSC-based metabolic therapies eventually reach clinical approval, whether they would accept previously banked tissue depends on their specific manufacturing and quality requirements, which do not yet exist. The adipose tissue banking guide explains exactly what banking preserves and what it does not provide.
How can I tell if a stem cell clinic’s diabetes claims are based on real research?
Ask for the ClinicalTrials.gov registration number (NCT number) for the specific protocol. Verify that number independently at ClinicalTrials.gov. Ask whether the FDA has issued an IND for the cell product being used. Ask whether the procedure is being offered as part of a registered, IRB-reviewed study or as a commercial service. Ask for specific published citations supporting the claims, and whether the clinic clearly discusses both the preliminary nature of the evidence and the existence of standard diabetes treatments as alternatives. Clinics that cannot answer all of these specifically are not operating within a legitimate research framework.
Where can I read more about ADSCs in metabolic disease from reputable sources?
The spear and shield review at PMC10066342 is the most comprehensive overview of how ADSCs interact with obesity and metabolic dysfunction. The Journal of Clinical Endocrinology and Metabolism review at academic.oup.com/jcem covers both type 1 and type 2 diabetes mechanisms. The PMC reviews on ADSC EVs in NAFLD (PMC9481107) and adipose EVs in obesity (PMC11853251) address the extracellular vesicle dimension specifically. The guide to clinical trials for regenerative medicine on this site explains how to find and evaluate registered trials.
Key Takeaways for People Living with Metabolic Disease
Living with obesity, type 2 diabetes, or fatty liver disease is demanding in ways that go beyond medical management. The appeal of a cell-based approach that might address root causes rather than just symptoms is understandable and reasonable. What patients deserve is an honest account of where the science is, not where advocates wish it were.
Save My Fat’s role is to explain how adipose-derived cells are being studied in metabolic disease based on peer-reviewed data, and to be honest about the gap between research and available treatment.
The current picture:
- ADSCs and adipose EVs clearly influence metabolism and inflammation in animal and cell models, sometimes in directions that worsen metabolic dysfunction and sometimes in directions that may improve it, depending on the experimental context.
- Small human studies of SVF or ADSCs in diabetes have generated preliminary signals but are early, uncontrolled, and not definitive evidence of safety or efficacy.
- NAFLD and NASH studies with ADSCs and EVs are primarily preclinical; human clinical use remains experimental and has not reached phase III investigation.
- Banking adipose tissue preserves a biological resource within a regulated framework. It does not replace proven metabolic therapies and does not guarantee access to future experimental ones.
Patients are encouraged to share this article with their endocrinologist or hepatologist as a starting point for discussion. For more on the science of adipose-derived cells, the patient’s guide to ADSCs provides foundational biology. For service information including the pricing page, providers page, and information on banking for family members, those resources are available on this site. The about page explains who Save My Fat is and the standards it holds itself to.
This article is for educational purposes only and does not constitute medical or legal advice. Legal and medical review including endocrinology and hepatology input is required before publication. Please consult your physician before making any decisions about metabolic disease treatment or research participation.
Last Updated: April 19, 2026