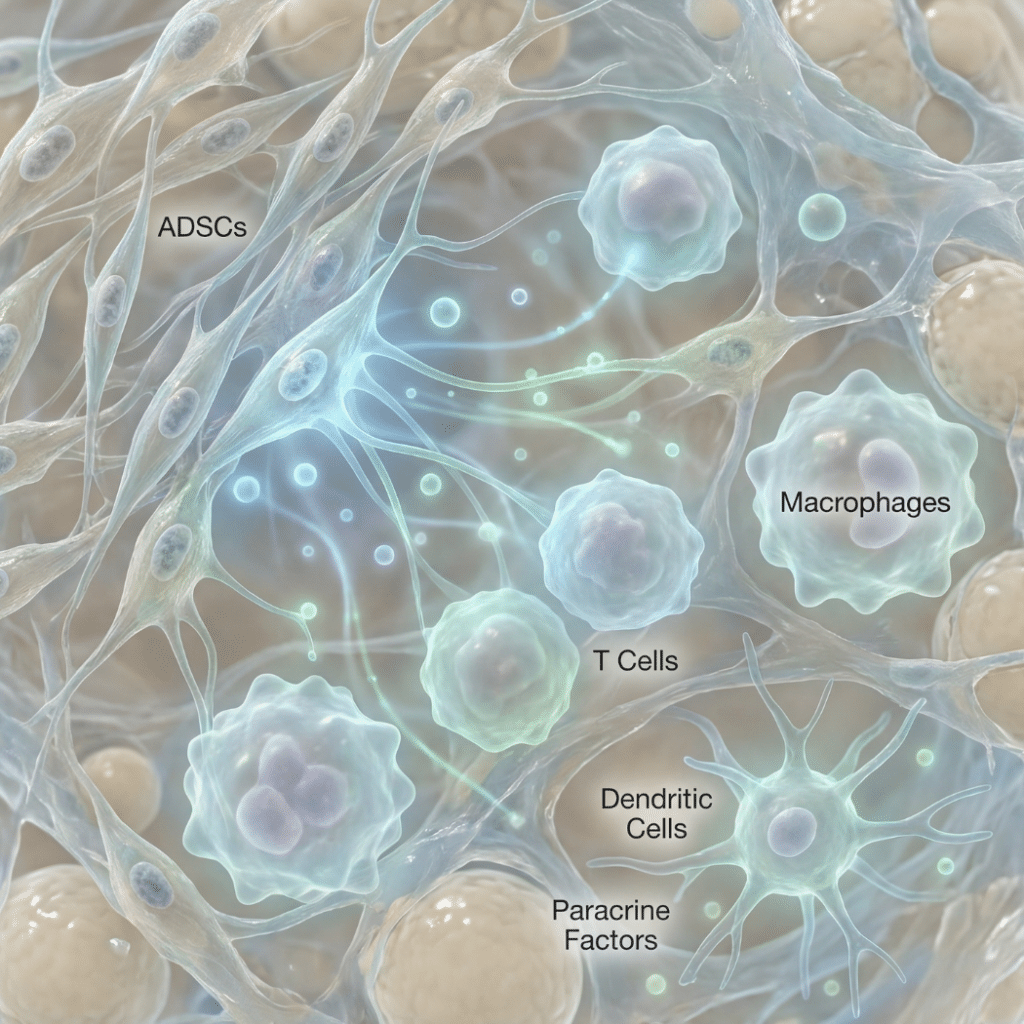
Adipose-derived stem cells are not just building blocks for new tissue. They also communicate actively with the immune system, releasing signaling molecules and interacting directly with immune cells in ways that researchers are still working to characterize. Scientists are exploring whether this immune modulation could eventually be useful in certain inflammatory and immune-mediated diseases, but most of that work is still in the research phase, ranging from laboratory experiments to early-stage clinical trials. Understanding what the science actually shows, and what it does not yet support, is the point of this guide.
TLDR: ADSCs release cytokines, growth factors, and extracellular vesicles that can reduce overactive immune responses in laboratory models and animal studies. They influence T cells, B cells, NK cells, macrophages, and dendritic cells through multiple molecular pathways. Some clinical trials are using MSCs (mesenchymal stromal cells) from various sources in conditions like graft-versus-host disease and autoimmune diseases, but these applications are investigational. Banking adipose tissue preserves a potential biological resource; it is not an immune therapy and does not provide immune modulation.
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease or medical condition. No adipose-derived stem cell product is FDA-approved to treat autoimmune diseases, graft-versus-host disease, or any other immune-mediated condition in the United States. This article explains immune modulation in research settings and does not constitute medical or legal advice. Patients must consult their own licensed healthcare professionals before considering any treatment or research study related to the immune system.
For many people living with chronic inflammation, autoimmune conditions, or other immune-mediated diseases, the idea of a therapy that could “calm” the immune system without the side effects of conventional immunosuppression sounds genuinely appealing. When they encounter the phrase “stem cells from fat can modulate the immune system,” the natural question is whether that claim reflects real science or is another piece of regenerative medicine marketing.
The answer is that the underlying science is real. There are peer-reviewed mechanistic studies, animal model data, and early human clinical experience showing that adipose-derived mesenchymal stromal cells (ADSCs, also called ASCs or adipose-derived MSCs) can influence immune cell behavior under certain conditions. The challenge is the distance between those research findings and a safe, effective, approved clinical therapy.
This guide walks through how ADSCs interact with the immune system at a biological level, what the published research says about the cells most affected, where clinical trials have tested these effects in humans, how exosomes fit into the picture, and what patients should understand when they encounter “immune modulation” claims in regenerative medicine marketing.
What “Immune Modulation” Means in Plain Language
Immune System Basics for This Conversation
The immune system has two major divisions. The innate immune system responds quickly to threats using cells like macrophages, natural killer (NK) cells, and dendritic cells. It does not have memory of specific pathogens. The adaptive immune system is slower but highly specific, using T cells and B cells that can recognize and remember particular targets. T cells can kill infected or abnormal cells, help other immune cells respond, or suppress immune reactions. B cells produce antibodies. Regulatory T cells (Tregs) are a specialized T-cell subset that help prevent the immune system from attacking the body’s own tissues.
In autoimmune diseases and chronic inflammatory conditions, immune regulation breaks down. The system targets the body’s own tissues (as in rheumatoid arthritis or lupus), maintains chronic inflammatory states (as in inflammatory bowel disease), or mounts exaggerated responses that cause collateral damage (as in severe graft-versus-host disease, or GVHD, following bone marrow transplantation). Therapies that can shift immune balance without broadly suppressing all immune function are highly sought after.
Where Mesenchymal Stromal Cells Fit
ADSCs are a type of mesenchymal stromal cell, a category of cells found in connective tissue throughout the body that have both tissue-supporting and immune-interacting properties. A 2020 review of the immunomodulatory effects of ADSCs, available at PMC7180192, describes how these cells secrete a range of cytokines, growth factors, and other signaling molecules that can influence immune cell behavior. Their immune effects do not depend primarily on the cells becoming new tissue; they arise from paracrine communication and direct cell-to-cell contact.
For a broader introduction to what ADSCs are and what properties make them biologically interesting, the patient’s guide to adipose-derived stem cells covers the foundational science.
Immunosuppression vs. Immunomodulation
These two terms are often used interchangeably but describe different things. Immunosuppression broadly reduces immune activity, as corticosteroids and chemotherapy do. This approach works but can leave patients vulnerable to infection and may have significant long-term effects.
Immunomodulation is more targeted: it aims to shift immune balance rather than globally suppress it. For ADSCs specifically, the mechanism of interest is not shutting the immune system down but adjusting it, for example by expanding regulatory T cells that promote tolerance, steering macrophages toward less inflammatory states, or reducing the activity of specific inflammatory mediators. A 2023 review of immunomodulatory functions of adipose mesenchymal stromal cells, published in Stem Cells Translational Medicine and accessible at academic.oup.com, describes this distinction in the context of adipose-derived cells specifically.
How Adipose-Derived Stem Cells Talk to Immune Cells
T Cells and Regulatory T Cells
T cells are among the immune cells most studied in the context of ADSC immunomodulation. In vitro experiments, meaning studies conducted in laboratory dishes rather than in living organisms, have consistently shown that ADSCs can inhibit the proliferation of activated T cells and promote the expansion of Tregs under inflammatory conditions. A 2021 Scientific Reports study examining immune modulation via adipose-derived MSCs, available at nature.com, describes several of the molecular mechanisms involved, including secretion of transforming growth factor beta-1 (TGF-beta-1), interleukin-6 (IL-6), and prostaglandin E2 (PGE2). Other mediators studied include indoleamine 2,3-dioxygenase (IDO), vascular cell adhesion molecule-1 (VCAM-1), and programmed death-ligand 1 (PD-L1), which interfere with T-cell activation through different pathways.
These in vitro findings are mechanistically coherent and reproducible across multiple research groups. They explain why researchers are interested in ADSCs for conditions where T-cell overactivity drives tissue damage. What in vitro data cannot show is whether the same magnitude of effect occurs in a living human with a specific immune condition, or whether it persists long enough to be clinically meaningful.
B Cells, NK Cells, and Dendritic Cells
ADSCs do not restrict their immune interactions to T cells. The 2020 immunomodulation review at PMC7180192 and an earlier 2013 review examining “Immunomodulatory Effects of Adipose-Derived Stem Cells: Fact or Fiction?” both describe effects on B cells, including reduced proliferation and altered antibody production in certain experimental models. NK cell cytotoxic activity, which is how these cells kill abnormal targets, is also affected: ADSCs can reduce NK cell killing capacity in co-culture experiments, which has implications for both immune disease management and for understanding potential long-term safety considerations in cell therapy.
Dendritic cells, which serve as the immune system’s primary antigen-presenting cells and help direct adaptive immune responses, are another ADSC target. In vitro data suggest ADSCs can interfere with dendritic cell maturation and reduce their ability to activate T cells, potentially contributing to immune tolerance. These effects are generally described as context-dependent: they appear most pronounced in inflammatory environments where the cells are being activated.
Macrophages and Inflammatory Balance
Macrophages exist on a functional spectrum. Loosely described, M1-polarized macrophages are pro-inflammatory and important for fighting infection, while M2-polarized macrophages are more associated with tissue repair and resolution of inflammation. This is an oversimplification of complex biology, but it captures the concept of interest in regenerative medicine research.
Published preclinical studies, including work described in the PMC7180192 review and a study examining ADSC-derived extracellular vesicle effects on macrophage polarization, describe ADSCs and their secreted vesicles as capable of shifting macrophages toward a more anti-inflammatory state in experimental models. This macrophage polarization effect is one reason ADSCs are being studied in inflammatory lung conditions and other settings where macrophage-driven inflammation plays a central role.
Are Adipose-Derived Cells Different from Other MSCs?
Comparing ADSCs to Bone Marrow MSCs
Bone marrow-derived MSCs have the longest research history in immune modulation, and much of what is known about MSC immunobiology comes from bone marrow studies. For adipose-derived cells specifically, some comparative studies have suggested that ADSCs may secrete higher levels of certain immunosuppressive cytokines under stimulated conditions compared with bone marrow MSCs, resulting in stronger in vitro suppression of T-cell proliferation in those experimental systems.
A review examining adipose-derived stem cells’ sources, differentiation capacity, and applications, published in a 2020 review accessible at sciencedirect.com, provides comparative context between adipose and bone marrow MSC immunomodulatory properties while noting that these comparisons depend heavily on the specific assays, cell passages, and stimulation conditions used. Results are not identical across all laboratories, and caution is warranted in drawing sweeping conclusions from any single comparison study.
Donor Health and Cell Potency
An important and sometimes underemphasized consideration in ADSC immune research is the influence of donor characteristics on cell function. ADSCs obtained from donors with obesity, type 2 diabetes, or chronic inflammatory conditions have been shown in experimental systems to display increased baseline expression of inflammatory markers and reduced immunosuppressive capacity compared with cells from metabolically healthy donors. The 2023 Stem Cells Translational Medicine review at academic.oup.com discusses this variability and its implications for clinical applications.
This matters practically because the same cell type, from different people, may not function identically. It raises questions about how donor screening and manufacturing processes will need to account for this variability in future therapeutic applications, whether for autologous use (cells from the patient’s own tissue) or allogeneic use (cells from a screened, healthy donor).
Where Immune Modulation Has Been Studied in Humans
Graft-Versus-Host Disease Experience with MSCs
The most clinically advanced use of MSC-based immune modulation is in graft-versus-host disease (GVHD), a serious and sometimes life-threatening complication of allogeneic hematopoietic stem cell transplantation (bone marrow or stem cell transplants from a donor), where donor immune cells attack the recipient’s tissues. A 2022 review of MSC clinical trials in GVHD, accessible at PMC8895864, summarizes the human trial experience, which has primarily used bone marrow-derived or umbilical cord-derived MSCs rather than adipose-derived cells.
The clinical picture from GVHD trials is encouraging but complex: some patients respond to MSC treatment, others do not, and the optimal timing, dose, and patient selection criteria remain under investigation. A 2023 Nature Reviews Immunology perspective on current MSC therapy for GVHD, available at nature.com, describes the field’s progress and the significant questions that remain, including whether the mechanisms observed in laboratory studies translate predictably to clinical outcomes.
It is important to note that Ryoncil (remestemcel-L), the first FDA-approved MSC product, is a bone marrow-derived allogeneic MSC product approved in December 2024 specifically for steroid-resistant acute GVHD in pediatric patients. It is not an adipose-derived product, and its approval does not extend to adipose-derived MSCs or to any other condition.
Autoimmune and Inflammatory Disorders
Beyond GVHD, MSCs from various sources have been studied in small clinical trials for conditions including Crohn’s disease, systemic lupus erythematosus (SLE), multiple sclerosis, and rheumatoid arthritis. These are largely single-center, early-phase studies, many without randomized control groups. Results have been mixed. None of these conditions currently have an FDA-approved MSC-based therapy.
For autoimmune conditions specifically, the trial landscape is still primarily in phase I and phase II. For context on what those phase designations mean in terms of evidence quality, the guide to clinical trials for regenerative medicine provides a patient-accessible explanation.
Where Adipose-Derived MSCs Fit Specifically
Some clinical protocols and early-phase studies have specifically used adipose-derived MSCs or SVF (stromal vascular fraction, the heterogeneous cell mixture obtained from enzymatically processed adipose tissue) in inflammatory and immune-mediated settings, including inflammatory bowel disease and kidney disease with inflammatory components. These uses are experimental, conducted under registered protocols with regulatory oversight. They are not general clinical practice and should not be interpreted as established treatments for those conditions. The emerging research page on this site tracks where adipose-derived cell research is currently most active.
Exosomes and Cell-Free Immunomodulatory Strategies
ADSC-Derived Exosomes in Immune Modulation
Exosomes are small membrane-bound vesicles that cells release as part of their normal activity. ADSC-derived exosomes carry microRNAs, proteins, and lipids that reflect their parent cell’s biology and can influence recipient cell behavior. A 2025 review of ADSC exosomes and immune modulation, accessible at PMC11830602, describes how these vesicles have been shown to reduce lung inflammation, affect macrophage polarization, and modulate T-cell responses in preclinical models.
The appeal of exosome-based approaches is that they might deliver some of the paracrine benefits of ADSCs without the complexity, logistical demands, and potential risks of live cell infusion. A cell-free product could potentially be stored, shipped, and administered more like a conventional drug.
Advantages and Outstanding Questions
Preclinical evidence for ADSC exosome immunomodulation is accumulating, but important questions remain unanswered: optimal dosing, delivery route, manufacturing consistency across batches, and long-term safety in living systems have not been fully characterized for any exosome-based immune product. No ADSC-derived exosome product is FDA-approved for any immune-mediated condition. These remain investigational approaches at various stages of preclinical and early clinical development.
What the Big Reviews Conclude
Consensus Themes
Multiple independent systematic reviews have reached broadly consistent conclusions about ADSC immunomodulatory properties. The review at PMC7180192, the 2021 Scientific Reports analysis, the 2023 Stem Cells Translational Medicine review, and a 2025 review of recent advances in ADSC biology all describe consistent laboratory findings: ADSCs and their secretome can suppress T-cell proliferation, promote Tregs, reduce inflammatory cytokine production, and shift macrophage states in experimental models. These effects appear across multiple immune cell types and under various inflammatory conditions.
What the reviews also consistently note is that laboratory findings do not automatically predict clinical outcomes. The transition from robust in vitro effects to reliable clinical benefit has proven more complex than early optimism suggested, in part because the in vivo environment of a living patient is far more complex than a laboratory dish.
Key Unanswered Questions
The most significant gaps identified across these reviews include optimal dosing and timing for immune indications, since the immune-modulating effects of MSCs are dynamic and influenced by the inflammatory environment; long-term safety, including whether immune suppression from ADSC therapy increases infection susceptibility or affects immune surveillance for tumors; and how donor characteristics and manufacturing variables translate into product potency consistency.
Regulatory and Clinical Status
Most ADSC immune modulation work remains in phase I or II trials. Regulatory agencies review each proposed product based on its specific manufacturing process, cell source, clinical indication, and submitted data. The general concept of immunomodulation does not earn regulatory approval; specific products with specific safety and efficacy data do. The field has not yet produced many ADSC-based immune products with the phase III data required for FDA consideration of approval.
What This Means for Patients and Tissue Banking
Banking Is Not an Immune Therapy
This is the most important practical clarification in this entire article. Banking adipose tissue through a service like Save My Fat stores a person’s intact tissue under validated cryopreservation conditions for potential future use. For what the banking process involves step by step, the adipose tissue banking guide and the how banking works article provide detailed explanations.
Banking does not provide immune modulation today. It does not connect a patient to any clinical trial or immune therapy currently in development. It does not make a patient eligible for any study. And it does not mean that the specific cell preparation methods used in immune research trials would be compatible with tissue banked through a consumer service.
Future Possibilities, Present Realities
The immune biology of ADSCs is one of the most scientifically compelling aspects of this field. It is reasonable to expect that research into MSC-based immune modulation, including adipose-derived approaches, will continue and that some products will eventually reach clinical approval for specific indications. Whether any future immune therapy would use banked adipose tissue, and under what specific conditions, is unknown today and will depend on trial designs and product specifications that do not yet exist.
Banking preserves a biological option within a compliant regulatory framework. It does not guarantee that any specific future immune application will be accessible, appropriate for a given patient, or compatible with previously banked material.
How to Interpret “Immune Modulation” Claims Online
When a clinic or website uses “immune modulation” in its marketing, the following questions are worth asking. Can they cite specific published studies with peer-reviewed citations and, ideally, PMC or PubMed identifiers? Does the therapy they are offering have a ClinicalTrials.gov registration number that can be independently verified? Is an IND in place for the cell product being used? Is the therapy described as experimental research, or is it being presented as a proven treatment? Broad claims about “resetting” or “rebooting” the immune system without specific mechanistic and regulatory substance should be evaluated with appropriate skepticism.
Frequently Asked Questions
What does it actually mean when a stem cell is “immunomodulatory”?
Immunomodulatory means the cell can influence how the immune system behaves, typically by releasing signaling molecules that affect other immune cells or by direct cell-to-cell contact. For ADSCs specifically, this involves secretion of cytokines including TGF-beta, IL-6, and PGE2, and expression of surface molecules like PD-L1 and IDO, that can reduce T-cell activation, promote regulatory T cells, and shift macrophages toward less inflammatory states in laboratory models. “Immunomodulatory” is a research description of cell behavior in experimental conditions; it does not mean the cell functions as an approved immune therapy in clinical practice.
Are adipose-derived stem cells better at immune modulation than bone marrow stem cells?
Some comparative studies suggest ADSCs may produce higher levels of certain immunosuppressive factors and show stronger in vitro T-cell suppression than bone marrow MSCs under some experimental conditions. However, these comparisons are sensitive to how the studies are designed, what passage number the cells are at, and what stimulation conditions are used. The differences are not consistently reproduced across all research groups, and neither adipose nor bone marrow MSCs have an established clinical superiority record in immune modulation at this stage of the science.
Can adipose-derived stem cells cure autoimmune diseases today?
No. Adipose-derived stem cells are not FDA-approved to treat any autoimmune disease, and their use in autoimmune contexts remains investigational. Small clinical trials have explored ADSCs and other MSC types in conditions like Crohn’s disease and lupus, but most are phase I or II studies and results have been mixed. The laboratory biology is scientifically compelling, but translating in vitro immunomodulatory effects into safe and effective clinical therapies has proven challenging across the MSC field broadly.
What human diseases are currently being studied with MSC-based immune therapies?
The most clinically advanced application is steroid-resistant acute GVHD, for which the bone marrow-derived MSC product Ryoncil received FDA approval in December 2024 for pediatric patients. Other conditions being investigated in clinical trials with various MSC sources, including adipose-derived cells in some cases, include Crohn’s disease, inflammatory bowel disease, lupus, multiple sclerosis, and kidney disease with inflammatory components. These applications are investigational; enrollment in a clinical trial is the appropriate route for patients interested in participating, not off-trial commercial services.
Do exosomes from adipose-derived cells count as immune therapies?
Not currently, and not in the regulatory sense. ADSC-derived exosomes have demonstrated immunomodulatory effects in preclinical models and are being investigated in early-stage research. No exosome-based immune therapy derived from adipose-derived cells is FDA-approved for any indication. Exosome research in immune modulation is active and scientifically interesting, but the manufacturing, dosing, and long-term safety questions that must be answered before regulatory approval remain open. Any clinic offering exosome-based immune treatments outside of a registered clinical trial is offering an unapproved product.
If I bank my fat now, does that mean I can later use it for immune-modulating treatments?
Not automatically. Banking preserves your adipose tissue in a compliant storage framework. Whether any future immune-modulating application would accept tissue banked through a consumer service depends on the specific product’s manufacturing requirements, clinical protocols, and regulatory approvals at that future time, none of which are defined today. Current MSC immune research primarily uses allogeneic products from donor sources or autologous products collected fresh as part of a specific trial protocol. Banking creates a biological resource; it does not create access to specific future applications.
How can I tell if a clinic’s “immune reset” treatment is based on real research?
Ask for the ClinicalTrials.gov registration number (NCT number) and verify it independently. Ask whether an IND is in place with the FDA for the cell product being used. Ask whether the treatment is being offered as part of a registered, IRB-reviewed study or as a commercial service. Ask for specific citations to peer-reviewed publications supporting the mechanism and safety of the product. “Immune reset,” “immune reboot,” and similar phrases without specific mechanistic or regulatory substance are warning signs. Legitimate researchers describe their work with precision and acknowledge limitations.
Where can I read more about ADSC immune effects from reputable sources?
The PMC7180192 review provides a comprehensive summary of immunomodulatory mechanisms. The 2023 Stem Cells Translational Medicine review covers immunomodulatory functions with attention to adipose-specific considerations. PMC8895864 reviews MSC clinical trials in GVHD for context on human applications. The guide to clinical trials for regenerative medicine on this site explains how to evaluate trial listings and research quality.
Key Takeaways for People Exploring Immune Modulation
Living with an immune-mediated condition or chronic inflammation drives many people to look beyond conventional treatments. The desire to understand whether regenerative medicine offers something different is reasonable, and the underlying science around ADSC immunomodulation is genuinely interesting.
Save My Fat’s role is to explain that immune science clearly and honestly, without overpromising what current research can support.
The practical picture:
- ADSCs clearly influence multiple immune cell populations in laboratory and animal studies through well-characterized molecular pathways.
- Early human trials suggest potential in certain immune-mediated diseases, but therapies from adipose-derived cells are not yet standard or widely approved.
- Exosomes and cell-free strategies add another dimension to this research field and remain experimental.
- Banking adipose tissue preserves a biological resource for potential future use. It is not an immune therapy and does not provide immune modulation.
For patients with immune-mediated conditions, the right place to discuss treatment options, including whether any clinical trial might be appropriate, is with a licensed specialist in rheumatology, immunology, or the relevant field. Research participation should be evaluated through registered trials with appropriate oversight.
To explore more about the science of adipose-derived cells and how the banking process fits into the larger regenerative medicine picture, the patient’s guide to adipose-derived stem cells, the emerging research page, the complete adipose tissue banking guide, and the how banking works article are starting points. For service information, the pricing page, providers page, and family page provide relevant details. The about page describes who Save My Fat is and how it approaches patient education.
This article is for educational purposes only and does not constitute medical or legal advice. Legal and medical review, including input from immunology and rheumatology specialists, is required before publication. Please consult your licensed healthcare provider regarding all treatment and research participation decisions.
Last Updated: April 17, 2026







