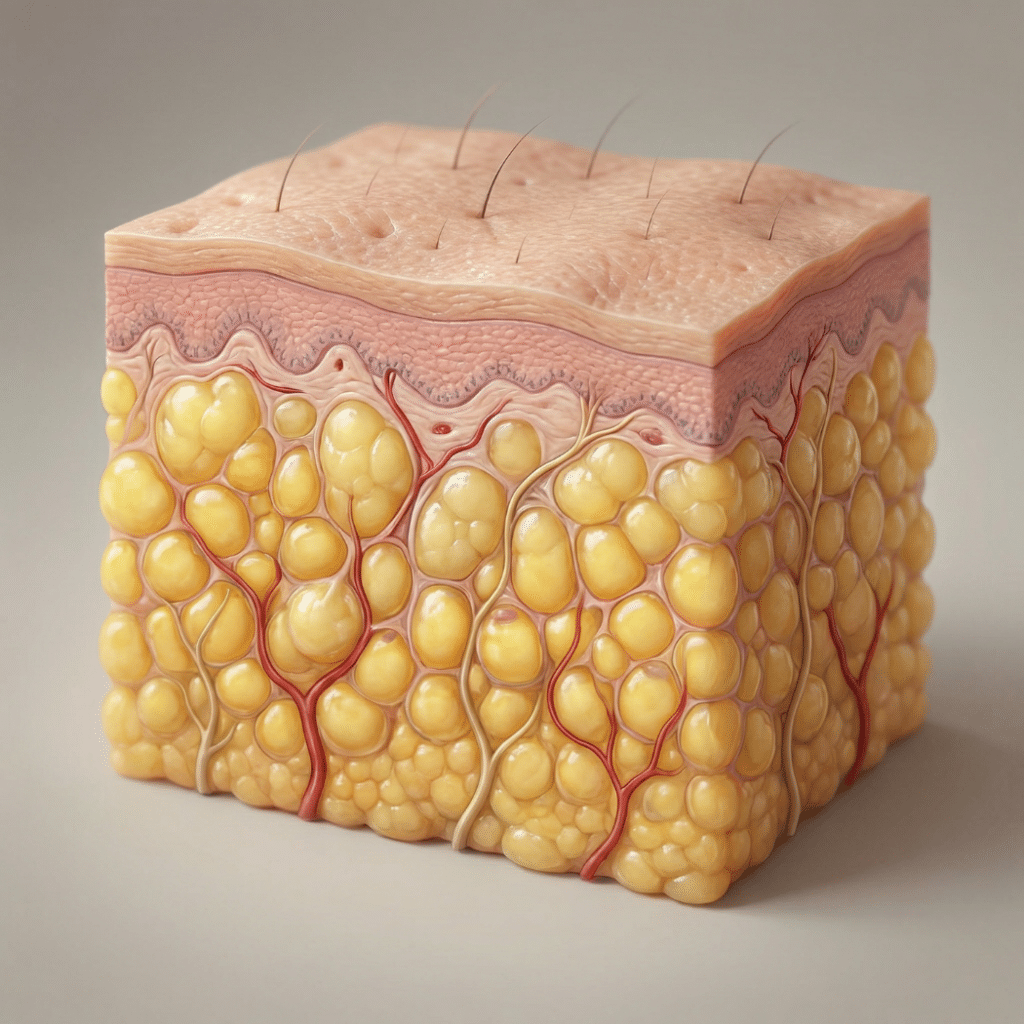
For most of the 20th century, scientists viewed body fat as a passive energy storage compartment, biologically inert tissue whose only role was to stockpile calories. That understanding changed dramatically starting in the 1990s with the discovery of leptin and the realization that adipose tissue is a complex, biologically active organ. This guide explores the science of fat from the inside out, covering its multiple cell types, its endocrine functions, its role as a stem cell reservoir, and why these properties matter for regenerative medicine research and tissue banking.
TLDR: Adipose tissue is not inert. It is a dynamic organ containing at least four types of fat cells (white, brown, beige, pink), a diverse population of non-fat cells including mesenchymal stem cells, and an extracellular matrix that functions as a stem cell niche. Adipose tissue produces hormones and signaling molecules that influence metabolism, immunity, and inflammation throughout the body. These biological properties are why researchers are studying adipose tissue for regenerative medicine applications, and why tissue banking preserves more than just “fat.”
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease. Banking adipose tissue does not guarantee eligibility, access, or clinical benefit from any future therapy, clinical trial, or medical program. All content is for educational purposes only and does not constitute medical advice. Patients must consult their own licensed healthcare professionals regarding all medical decisions.
If someone told you that the fat on your abdomen is a sophisticated endocrine organ that produces hormones, contains stem cells, and communicates with your brain, heart, and immune system, you might be skeptical. But that is exactly what published research has demonstrated over the past three decades.
Adipose Tissue Is Not Just Fat
The paradigm shift began in 1994, when Jeffrey Friedman’s laboratory at Rockefeller University discovered leptin, a hormone produced almost exclusively by fat cells. This single discovery upended the prevailing assumption that adipose tissue was hormonally inert. It demonstrated that fat cells actively communicate with the brain to regulate appetite and energy balance.
Since then, researchers have identified dozens of signaling molecules secreted by adipose tissue, collectively called adipokines. These molecules influence metabolism, insulin sensitivity, cardiovascular health, immune function, brain function, and reproduction (Ronti et al., 2006; Scherer, 2006).
Modern science now recognizes adipose tissue as one of the largest endocrine organs in the body. It is not just sitting there. It is an active participant in nearly every major physiological system (Endotext, 2020).
The Four Types of Adipocytes
Body fat is not a single, uniform substance. Researchers have identified at least four distinct types of adipocytes, each with different structures, functions, and locations.
Adipocyte Types
| Adipocyte Type | Appearance | Primary Function | Location | Key Feature |
|---|---|---|---|---|
| White | Large single lipid droplet, few organelles | Energy storage, endocrine signaling | Subcutaneous, visceral (largest depots) | Produces leptin, adiponectin, resistin; largest adipose volume in adults |
| Brown | Multiple small lipid droplets, many mitochondria | Thermogenesis (heat generation) | Interscapular, supraclavicular, paravertebral | Contains UCP-1 (uncoupling protein-1); iron-rich mitochondria give brown color |
| Beige (brite) | Intermediate characteristics | Thermogenesis when activated (“browning”) | Interspersed within subcutaneous WAT | Arises from white adipocyte conversion or distinct preadipocytes; activatable by cold, exercise |
| Pink | Transformed from white during pregnancy/lactation | Milk production | Mammary gland (pregnancy) | Most recently discovered; demonstrates extreme adipocyte plasticity |
Sources: Endotext, 2020; Frontiers in Physiology, 2018; A Palette of Adipose Tissue, 2021
White adipocytes make up the vast majority of adult body fat. They store triglycerides in a single large lipid droplet and serve as the body’s primary long-term energy reserve. Critically, they are also the primary source of adipokines.
Brown adipocytes generate heat through a process called non-shivering thermogenesis, using a specialized mitochondrial protein called UCP-1. Once thought to exist only in infants, research has confirmed that adults retain functional brown adipose tissue in specific anatomical locations.
Beige adipocytes are particularly interesting. These cells develop within white adipose tissue and can be activated by cold exposure, exercise, and certain hormones to take on brown-like, heat-generating characteristics. This “browning” process is an active area of metabolic research (MDPI, 2025).
Pink adipocytes are the most recently described type, arising from white adipocytes during pregnancy and lactation to support milk production. Their existence demonstrates what researchers call the “extraordinary plasticity” of adipose tissue: the ability of fat cells to transform their identity in response to physiological demands.
Where Fat Lives: Subcutaneous vs. Visceral Adipose Tissue
Not all fat depots are biologically equivalent. Where fat is located in the body has a significant impact on its metabolic behavior and health implications.
Subcutaneous vs. Visceral Adipose Tissue
| Parameter | Subcutaneous (SAT) | Visceral (VAT) |
|---|---|---|
| Location | Beneath the skin (abdomen, thighs, hips, arms) | Around internal organs (omentum, mesentery) |
| Proportion | ~80% of total body fat in lean individuals | ~10-20% in lean individuals |
| Metabolic profile | May retain protective features in early obesity | Critical site of inflammation and metabolic inflexibility |
| Adipokine profile | Higher adiponectin (anti-inflammatory) | Higher pro-inflammatory cytokines (IL-6, TNF-alpha) |
| Disease association | Lower metabolic risk per volume | Strongly associated with insulin resistance, cardiovascular disease, type 2 diabetes |
| Stem cell content | High MSC yield (2-5 x 10^5 SVF cells/mL from abdomen) | SVF composition differs; more inflammatory cell infiltration |
| Harvest for banking | Primary source (abdomen, flanks, thighs) | Not typically harvested |
Sources: MDPI, 2025; Endotext, 2020; SVF characterization across depots, 2017
The fat under your skin (subcutaneous fat), particularly from the abdomen and flanks, is the type that is harvested for tissue banking. It is metabolically different from the deep visceral fat around your organs. This is also where the highest concentration of adipose-derived stem cells resides. Learn more about how tissue collection works on the how stem cell banking works page.
Fat as an Endocrine Organ: What Adipose Tissue Communicates
Adipose tissue produces and secretes a family of signaling molecules called adipokines. These chemical messengers act locally within the tissue and travel through the bloodstream to affect distant organs (Ronti et al., 2006).
Key Adipokines and Their Functions
| Adipokine | Produced By | Primary Functions | Clinical Relevance |
|---|---|---|---|
| Leptin | White adipocytes (proportional to fat mass) | Appetite regulation, energy balance, reproductive function, immune signaling | Leptin resistance is a hallmark of obesity; elevated levels associated with cardiovascular risk |
| Adiponectin | White adipocytes (inversely proportional to fat mass) | Insulin sensitization, anti-inflammatory, cardioprotective, fatty acid oxidation | Low levels associated with metabolic syndrome, type 2 diabetes, cardiovascular disease |
| Resistin | White adipocytes and immune cells | Implicated in insulin resistance (role in humans less clear than in rodents) | Elevated in inflammatory conditions |
| TNF-alpha | Adipose tissue macrophages | Pro-inflammatory cytokine; contributes to insulin resistance | Elevated in obesity; linked to chronic low-grade inflammation |
| IL-6 | Adipocytes and SVF cells | Dual role: pro-inflammatory systemically, may have local anti-inflammatory effects | Elevated in visceral obesity; linked to cardiovascular risk |
| Estrogen | Adipose tissue aromatase | Converts androgens to estrogen | Relevant in post-menopausal health |
| PAI-1 | Adipocytes | Inhibits blood clot breakdown (fibrinolysis) | Elevated in obesity; contributes to thrombotic risk |
Sources: Ronti et al., 2006; Adipokines in Health and Disease, 2023; Endotext, 2020
Fat is actively communicating with the brain (appetite), the pancreas (insulin sensitivity), the heart (cardiovascular health), the immune system (inflammation), and the reproductive organs (hormones) through these chemical signals. This communication network is why maintaining healthy adipose tissue function matters, and it is one reason that preserving adipose tissue with its full cellular ecosystem has biological rationale for researchers.
Beyond Adipocytes: The Cellular Ecosystem Inside Adipose Tissue
Fat cells (adipocytes) make up the majority of adipose tissue by volume, but they are not the majority by cell count. The non-adipocyte cells collectively make up the stromal vascular fraction (SVF), a cellular concentrate that includes mesenchymal stem cells (15 to 30%), endothelial cells (10 to 20%), pericytes (3 to 5%), and various immune cells including granulocytes, monocytes, and lymphocytes (Bourin et al., 2013).
For a detailed breakdown of SVF composition, isolation methods, and regulatory status, see the companion guide: What Is SVF?
The adipose-derived stem cells (ADSCs) within this ecosystem are particularly notable for their secretome: the collection of bioactive molecules they release. Published research has identified ADSC-secreted factors including VEGF (vascular endothelial growth factor), HGF (hepatocyte growth factor), IGF-1, FGF-2, TGF-beta, and multiple neurotrophic factors. ADSCs also produce exosomes, tiny extracellular vesicles (30 to 150 nanometers) that carry proteins, lipids, and nucleic acids as a form of cell-to-cell communication (ADSC applications and future directions, 2020).
The diversity of this cellular ecosystem is why researchers view adipose tissue as more than just a source of stem cells. It is an integrated biological system.
The Extracellular Matrix: The Scaffold That Holds It All Together
Adipose tissue contains a collagen-rich extracellular matrix (ECM) that provides structural support and biological signaling to the cells embedded within it. The ECM is not inert scaffolding. It actively influences stem cell behavior, including differentiation, proliferation, and quiescence (the dormant state that helps preserve stem cell properties).
Research published in 2022 documented that the cell-cell communication within the adipose niche, orchestrated by the ECM and its resident cells, plays a crucial role in adipose tissue development, function, turnover, and remodeling (Adipose tissue in communication, 2022).
Recent research (2025) has demonstrated that adipose tissue-derived ECM can serve as hydrogel scaffolds for stem cell differentiation, showing that the matrix itself, not just the cells, has biological value (ECM hydrogels, 2025).
When adipose tissue is cryopreserved for banking, both the cells and the ECM are preserved together. This approach maintains the niche environment rather than isolating cells from their native context. For details on how cryopreservation works, see: How Cryopreservation Works.
How Adipose Tissue Changes with Age
Adipose tissue biology does not remain constant throughout life. Published research has documented several age-related changes that affect both the tissue’s metabolic function and its regenerative properties.
Fat redistribution is one of the most visible changes: subcutaneous fat tends to decrease while visceral fat increases, shifting the body’s adipose profile toward a more inflammatory state (Aging adipose, 2021).
At the cellular level, aging is associated with increased inflammation (sometimes called “inflammaging”), the accumulation of senescent cells that no longer divide, impaired thermogenesis as brown and beige fat function declines, increased fibrosis of the ECM, and a gradual decline in ADSC regenerative potential. Published research describes this as “a multifaceted process driven by diverse mechanisms, involving dysregulated adipogenic pathways, impaired thermogenesis, reduced regeneration, onset of senescence, and emergence of inflammation” (Adipose tissue aging, 2022).
However, an important nuance: published research suggests that ADSCs are more resilient to age-related decline than bone marrow-derived mesenchymal stem cells. ADSCs maintain differentiation capacity through multiple passages and can achieve over 50 population doublings. Age-related decline occurs, but studies comparing stem cell sources consistently show that adipose tissue retains higher yield and function across age ranges. These changes vary by individual, and more research continues to accumulate.
This is part of the scientific rationale for banking tissue earlier rather than later, preserving it at the donor’s current biological age for potential future use. For context on this topic, visit the wellness and healthy aging page. For comparison with bone marrow stem cells, see the companion guide.
Important: Banking does not guarantee access to any treatment, clinical trial, or medical program.
Why This Biology Matters for Regenerative Medicine
The biological properties described throughout this article are why adipose tissue has become a focus of regenerative medicine research. Its unique combination of characteristics includes high stem cell yield (approximately 500 times more MSCs per gram than bone marrow), minimally invasive harvest through liposuction under local anesthesia, a rich secretome and exosome production profile, endocrine and immunomodulatory functions, availability at any adult age (unlike birth tissue sources, which have a single collection window), and autologous use (your own cells, eliminating immune rejection concerns).
Hundreds of clinical trials involving ADSCs are registered on ClinicalTrials.gov. Research areas span orthopedics, cardiovascular, neurological, autoimmune, wound healing, and metabolic conditions. No adipose-derived stem cell products are currently FDA-approved for disease treatment. Clinical trials are research studies, not treatment programs.
For more on the research landscape, visit the emerging research page and the joint and orthopedic research page. For a comparison with birth tissue stem cell sources, see the companion guide.
What This Means for Tissue Banking
When adipose tissue is banked through cryopreservation, the process preserves the complete biological system: white adipocytes and their ECM scaffold, the full stromal vascular fraction (including ADSCs, endothelial cells, pericytes, and immune cells), the extracellular matrix niche environment, and the secretome and exosome-producing capacity of those cells. All of this is preserved at the donor’s current biological age for potential future use in FDA-regulated clinical pathways.
Learn more about the banking process at the complete guide to adipose tissue banking. For pricing information or to find a provider, visit those pages. First-degree family members may potentially qualify to use banked cells under certain guidelines; visit the family page for details.
Important: Banking does not guarantee access to any treatment, clinical trial, or medical program. All future use would require proper regulatory authorization.
Frequently Asked Questions
What is adipose tissue? Adipose tissue is the scientific name for body fat. It is a specialized connective tissue composed primarily of fat cells (adipocytes) along with a supporting network of stem cells, blood vessel cells, immune cells, and extracellular matrix. It is now recognized as a major endocrine organ.
Is all body fat the same? No. Researchers have identified at least four types of adipocytes (white, brown, beige, and pink), each with distinct functions. Fat also varies significantly by location: subcutaneous fat (under the skin) behaves differently from visceral fat (around internal organs).
What is brown fat, and do adults have it? Brown adipose tissue generates heat through a process called thermogenesis. Once thought to exist only in infants, research has confirmed that adults retain functional brown fat in specific locations including the neck, collarbone area, and along the spine. Brown fat activity tends to decline with age.
Is subcutaneous fat healthier than visceral fat? Published research indicates that subcutaneous fat may retain protective metabolic features, particularly in early obesity, while visceral fat is more strongly associated with inflammation, insulin resistance, and cardiovascular disease risk. The subcutaneous depot is also the primary source for adipose tissue banking due to its higher stem cell content and easier access.
What hormones does fat produce? Adipose tissue produces leptin (appetite regulation), adiponectin (insulin sensitization), resistin, estrogen, and various inflammatory cytokines including TNF-alpha and IL-6. These adipokines influence metabolism, cardiovascular health, immune function, and reproductive biology.
What is the difference between adipocytes and adipose-derived stem cells? Adipocytes are the mature fat cells that store energy. Adipose-derived stem cells (ADSCs) are a different cell population within the tissue’s stromal vascular fraction. ADSCs are multipotent progenitor cells that can differentiate into multiple cell types in laboratory settings.
Does fat quality change with age? Published research documents age-related changes including redistribution from subcutaneous to visceral depots, increased inflammation, accumulation of senescent cells, and gradual decline in stem cell function. However, ADSCs appear more resilient to aging than bone marrow-derived stem cells.
Why is adipose tissue studied for regenerative medicine? Adipose tissue yields approximately 500 times more mesenchymal stem cells per gram than bone marrow, can be harvested through minimally invasive liposuction, is available at any adult age, and is autologous (the patient’s own tissue). These properties have made it a focus of hundreds of clinical trials across multiple research areas.
What happens to adipose tissue when it is cryopreserved? Cryopreservation uses protective agents and controlled cooling rates to preserve the tissue and its cells at ultra-low temperatures. Published research shows post-thaw viability rates of 80 to 91% using standard protocols. See the companion guide: How Cryopreservation Works.
Can I bank adipose tissue at any age? Adipose tissue can be collected from adults at any age, which is a significant advantage over birth tissue sources that have a single collection window at delivery. However, banking earlier preserves tissue at a younger biological age. All medical decisions should be made with a licensed healthcare provider.
Key Takeaways
Fat Is a Dynamic Organ, Not Passive Storage
- Adipose tissue produces hormones, communicates with the brain, heart, and immune system, and contains at least four types of specialized cells
Location Matters
- Subcutaneous fat (under the skin) behaves differently from visceral fat (around organs) and is the primary source for tissue banking
Adipose Tissue Contains an Entire Cellular Ecosystem
- Beyond fat cells, the tissue houses stem cells, blood vessel cells, immune cells, and a biologically active extracellular matrix
These Properties Drive Research Interest
- High stem cell yield, minimally invasive harvest, rich secretome, and autologous availability make adipose tissue a focus of regenerative medicine research
Biology Changes with Age
- Age-related decline affects adipose tissue function and stem cell properties, though ADSCs appear more resilient than bone marrow stem cells
Banking Preserves the Complete System
- Cryopreservation preserves the cells, the matrix, and the niche environment together at the donor’s current biological age
Learn More About Adipose Tissue Banking
Before contacting Save My Fat: Adipose tissue banking is a preservation service for potential future opportunities, not a treatment or cure for any disease. Outcomes cannot be guaranteed. All medical decisions must be made with a licensed healthcare provider.
Visit the how stem cell banking works page for an overview of the collection process.
For the complete guide, see What Is Adipose Tissue Banking?.
Healthcare providers can visit the providers page.
Learn about Save My Fat at the about page.
Last updated: March 11, 2026







