If you have ever wondered what makes body fat more than just stored energy, you are not alone. Scientists have found that fat tissue holds a surprising number of special cells called stem cells, and researchers around the world are studying them. This guide explains what adipose-derived stem cells are, where they come from, how they compare to other stem cell types, and what this means for people thinking about adipose tissue banking.
TLDR: Adipose-derived stem cells (ADSCs) are adult stem cells found inside your body fat. Fat tissue can contain 100 to 1,000 times more of these cells per gram than bone marrow, making it one of the richest known sources. No ADSC-based therapy is FDA-approved today. Banking your adipose tissue preserves these cells at their current biological age for potential future use, but banking does not guarantee access to any treatment or clinical trial. Read on to learn the science in simple terms.
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease. Banking adipose tissue today does not guarantee eligibility, access, or clinical benefit from any future therapy, clinical trial, or medical program. All content is for educational purposes only and does not constitute medical advice. Patients must consult their own licensed healthcare professionals regarding all medical decisions.
You have probably heard the word “stem cells” in the news or from a friend. Maybe a doctor mentioned them, or you saw an ad from a clinic making big promises. The problem is that a lot of information out there mixes real science with hype.
This guide breaks down the science of fat-derived stem cells in plain language. You will learn what these cells are, why scientists are excited about them, and what the current rules say about using them. You will also learn how adipose tissue banking fits into the picture and why it is not the same thing as getting a treatment.
What Is Adipose Tissue?
Adipose tissue is the medical term for body fat. Most people think of fat as something they want to lose, but fat actually plays many important roles in the body. It does far more than just store extra calories.
More Than Energy Storage
Fat tissue works like a small organ. It sends chemical signals to the rest of the body, helps control hunger, and plays a role in how the body fights infection. Scientists call it an endocrine organ (a part of the body that makes and sends out hormones) because of all the messages it sends to other cells (Baer & Geiger, 2012).
Two Main Types of Fat
White adipose tissue makes up most of your body fat. It stores energy, cushions your organs, and keeps you warm. Brown adipose tissue is less common and mainly produces heat. Most stem cells that scientists study come from white adipose tissue, which is the type collected during adipose tissue banking.
A Mix of Different Cells
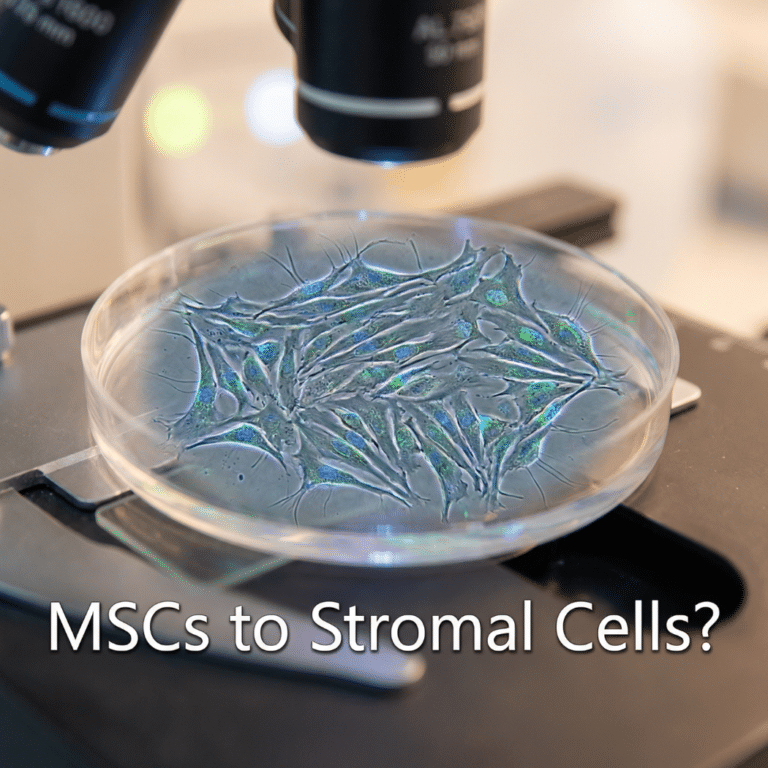
Fat tissue is not just fat cells. It also contains blood vessel cells, immune cells, connective tissue cells, and stem cells. The fat cells themselves (called adipocytes, pronounced AD-ih-po-sites) make up only part of the total cell population. This mix of other cells is where adipose-derived stem cells are found (Chu et al., 2019).
What Are Adipose-Derived Stem Cells (ADSCs)?
Adipose-derived stem cells, often called ADSCs or ASCs, are a type of adult stem cell found inside your body fat. They belong to a larger family of cells called mesenchymal stem cells (MSCs), which are sometimes called mesenchymal stromal cells.
What Are Mesenchymal Stem Cells?
Mesenchymal stem cells (pronounced mez-EN-kih-mal) are adult stem cells with two key abilities. First, they can make copies of themselves (self-renewal). Second, they can develop into several different types of cells, including fat cells, bone cells, and cartilage cells. Scientists call this multilineage differentiation potential (Bunnell et al., 2008).
The word “adult” is important. ADSCs are not embryonic stem cells. They come from a grown person’s body, not from an embryo.
How Scientists Identify ADSCs
An international group of scientists from IFATS and ISCT published a joint statement defining what counts as a mesenchymal stem cell. The cells must (Bourin et al., 2013):
- Stick to plastic surfaces in the lab (plastic adherence)
- Show specific surface markers: more than 95% must express CD73, CD90, and CD105, while less than 2% express CD14, CD34, CD45, or HLA-DR
- Turn into three cell types in lab conditions: fat cells (adipogenic), bone cells (osteogenic), and cartilage cells (chondrogenic), known as trilineage differentiation
What Is the Stromal Vascular Fraction (SVF)?
When scientists or doctors process fat tissue in a lab, they separate it into two parts. The mature fat cells (adipocytes) float to the top and are removed. Everything else that remains is called the stromal vascular fraction, or SVF (Bourin et al., 2013).
What Is Inside SVF?
SVF is a mix of many different cell types. It is not a single kind of cell. The mixture typically includes:
- ADSCs/MSCs (the stem cells)
- Endothelial progenitor cells (young blood vessel cells)
- Pericytes (cells that wrap around small blood vessels)
- Fibroblasts (connective tissue cells)
- Immune cells (such as macrophages and lymphocytes)
- Red blood cells
Think of SVF like a fruit salad: it contains many ingredients mixed together, and the stem cells are just one of those ingredients (Gimble et al., 2013).
How ADSCs Are Separated from SVF
To get a more concentrated population of stem cells, scientists place SVF cells in lab dishes. The ADSCs stick to the plastic surface while other cell types do not. Over time, the ADSCs grow and multiply, and the non-sticky cells are washed away. This is called plastic-adherent culture selection (Bunnell et al., 2008).
Freshly collected SVF cells carry different surface markers than ADSCs that have been grown in culture. Scientists use “ASCs” for the culture-expanded version and “SVF cells” for the freshly isolated mix (Bourin et al., 2013).
Regulatory note: SVF that has been processed through enzymatic digestion is generally classified by the FDA as more than minimally manipulated. This means it falls under the Section 351 regulatory pathway, which requires clinical trials and FDA approval before it can be marketed for any disease treatment. No SVF-based therapy is currently FDA-approved (21 CFR Part 1271).
Why Is Fat Considered a Rich Source of Stem Cells?
One of the biggest reasons researchers are interested in adipose tissue is the sheer number of stem cells it contains compared to other sources.
Cell Yield: Fat vs. Bone Marrow
Published research shows that fat tissue yields roughly 100 to 1,000 times more mesenchymal stem cells per gram than bone marrow (Bunnell et al., 2008). That is a very large difference. For perspective, one gram of fat tissue can produce approximately 5,000 stem cells, while one gram of bone marrow typically produces far fewer (Locke et al., 2009).
Other Advantages of Adipose Tissue as a Source
Fat tissue has several practical benefits as a stem cell source:
- Abundance: Most adults carry a meaningful amount of subcutaneous fat (fat under the skin) that can be collected
- Accessibility: Collection uses a minimally invasive mini-liposuction procedure, which is generally less uncomfortable than a bone marrow aspiration
- Proliferation: ADSCs from fat tissue show strong ability to multiply in lab settings, meaning a small starting sample can grow into a larger supply (Chu et al., 2019)
Comparison Table: Adipose Tissue vs. Bone Marrow
The following table compares these two stem cell sources based on published research:
| Feature | Adipose Tissue | Bone Marrow |
|---|---|---|
| MSC yield per gram | ~5,000 cells per gram (varies by donor) | 100 to 1,000 times fewer per gram |
| Harvesting method | Mini-liposuction under local anesthesia | Needle aspiration into hip bone, typically under sedation |
| Patient comfort | Generally well-tolerated | Can involve significant discomfort |
| Tissue availability | Abundant in most adults | Limited volume per session |
| Proliferation in culture | Robust proliferative capacity | Slower proliferation in some studies |
Sources: Bunnell et al., 2008; Iyyanki et al., 2015; Locke et al., 2009
Both tissue sources are subjects of ongoing study, and neither has produced an FDA-approved mesenchymal stem cell therapy.
How Are ADSCs Different from Bone Marrow Stem Cells?
Both adipose-derived stem cells (ADSCs) and bone marrow-derived stem cells (BMSCs) are types of mesenchymal stem cells. They share many features, but they are not identical.
Key Differences
Published research has found that ADSCs and BMSCs differ in several ways (Gimble et al., 2013):
- Surface markers: Both meet the basic MSC criteria, but they show some differences in the specific proteins on their surface
- Paracrine profiles: The signaling molecules each cell type releases (the chemical messages they send to nearby cells) can differ
- Differentiation tendencies: Some studies suggest ADSCs may lean more toward becoming fat cells, while BMSCs may lean more toward becoming bone cells
Collection Differences
ADSCs come from fat tissue collected through a mini-liposuction procedure using local anesthesia. BMSCs come from bone marrow, which requires a needle inserted into the hip bone. Many patients find the fat collection process more comfortable (Iyyanki et al., 2015).
For a deeper side-by-side comparison of these two stem cell sources, including what the latest research says, look for the upcoming companion article on bone marrow versus adipose-derived stem cells on the Save My Fat emerging research page.
How Are ADSCs Different from Birth Tissue Stem Cells?
Another common question is how fat-derived stem cells compare to stem cells from birth tissues like umbilical cord blood, Wharton’s Jelly, or amniotic fluid.
Autologous vs. Allogeneic
The biggest difference is where the cells come from. ADSCs collected from your own fat are autologous (aw-TAH-luh-gus), meaning they come from your own body. Birth tissue products are allogeneic (al-oh-jeh-NAY-ik), meaning they come from a donor, typically the mother and baby after delivery.
What Is Actually FDA-Approved?
This is a critical point. The FDA states that the only FDA-approved stem cell products in the United States consist of blood-forming stem cells (hematopoietic progenitor cells) from umbilical cord blood, approved only for certain blood disorders. No other stem cell product is FDA-approved for treating any disease.
No exosome products are FDA-approved. The FDA has issued a consumer alert warning about unapproved regenerative medicine products, including exosomes.
A Caution About Marketing Claims
Many clinics market birth tissue products as “stem cell treatments.” Published research has raised questions about how many viable stem cells actually survive the processing and freezing of these products. Patients should verify all claims with their healthcare provider before pursuing any product marketed as a stem cell treatment.
For a detailed comparison of birth tissue products and adipose-derived cells, watch for the upcoming companion article on the Save My Fat blog.
What Are Researchers Studying ADSCs For?
Scientists around the world are actively studying adipose-derived stem cells in clinical trials. It is important to understand that all of these studies are investigational, meaning they are testing whether something might work. None of these research areas have produced an FDA-approved ADSC-based therapy.
Areas of Active Research
Registered clinical trials on ClinicalTrials.gov are investigating ADSCs in areas that include:
- Orthopedic and musculoskeletal conditions: Researchers are studying whether ADSCs may play a role in joint, bone, and cartilage research. For example, one registered trial is examining SVF injection in knee osteoarthritis. These studies are research, not available treatments (Berman et al., 2018).
- Wound healing: Some studies are exploring how ADSCs and their signaling molecules may relate to tissue repair processes (Mazini et al., 2019)
- Autoimmune conditions: Early-stage research is examining the potential relationship between ADSCs and immune system function
This research is preliminary and does not prove that ADSCs are safe or effective for treating any condition. More studies are needed before any conclusions can be drawn. No FDA-approved treatments exist for these uses based on this research alone.
Patients who want to explore current studies can search ClinicalTrials.gov directly. A listing on ClinicalTrials.gov does not mean the product is proven safe, effective, or FDA-approved. Clinical trials are research studies, not treatment programs.
For more on what is being studied, visit the Save My Fat emerging research page and the pages on joint and orthopedic research and wellness and healthy aging.
How Does This Relate to Adipose Tissue Banking?
Understanding what ADSCs are helps explain why some people choose to preserve their fat tissue now, even though no ADSC-based treatments are FDA-approved today.
What Banking Does
Adipose tissue banking preserves your own fat tissue, and the ADSCs within it, through a process called cryopreservation (cry-oh-prez-er-VAY-shun). This means the tissue is carefully cooled and stored at extremely low temperatures in a specialized facility.
Cells banked today are preserved at their current biological age. Published research shows that adipose tissue can be cryopreserved for years with meaningful viability retention. Some studies report 80 to 91 percent post-thaw viability rates after eight or more years of storage (Chu et al., 2019). For a deeper look at the cryopreservation process, read the complete guide to adipose tissue banking.
What Banking Does Not Do
Banking adipose tissue does not guarantee access to any treatment, clinical trial, or medical program. It does not mean a therapy will be available, that a patient will be eligible for a study, or that stored cells will produce any clinical benefit. The future regulatory landscape for regenerative medicine is uncertain, and therapies that are investigational today may never receive FDA approval.
What banking does create is the option to have your own tissue available if legitimate medical opportunities arise, such as FDA-approved therapies, clinical trials, Expanded Access programs, or Right to Try pathways (where specific eligibility requirements apply).
Family Considerations
First-degree family members may potentially be eligible to use banked cells under certain guidelines. This makes adipose tissue banking a decision that could involve your broader family’s health planning. Eligibility depends on multiple factors and is not guaranteed.
Before You Contact Save My Fat: Adipose tissue banking is a preservation service for potential future opportunities, not a treatment or cure for any disease. Outcomes cannot be guaranteed. All medical decisions must be made with a licensed healthcare provider. Banking does not guarantee access to any therapy, clinical trial, or Expanded Access program.
Frequently Asked Questions
What are adipose-derived stem cells? Adipose-derived stem cells (ADSCs) are adult mesenchymal stem cells found in body fat. They can self-renew and develop into fat, bone, and cartilage cells in lab conditions. They are not embryonic stem cells. Learn more on the Save My Fat about page.
What is SVF (stromal vascular fraction)? SVF is the mix of cells left after mature fat cells are removed from processed adipose tissue. It contains stem cells, blood vessel cells, immune cells, and other cell types. Processing SVF through enzymatic digestion generally falls under the FDA’s 351 regulatory pathway.
How many stem cells are in fat tissue? Published research suggests fat tissue yields roughly 100 to 1,000 times more mesenchymal stem cells per gram than bone marrow. The exact number varies by donor age, harvest site, and collection method (Iyyanki et al., 2015).
Are fat stem cells the same as bone marrow stem cells? Both are mesenchymal stem cells, but they come from different tissues and show differences in surface markers, signaling profiles, and differentiation tendencies. Fat harvesting is generally less invasive than bone marrow aspiration.
Are adipose-derived stem cells the same as embryonic stem cells? No. ADSCs are adult stem cells from a person’s own body fat. Embryonic stem cells come from embryos. They are fundamentally different cell types with different ethical and regulatory considerations.
Is it painful to collect adipose tissue for banking? Collection uses a minimally invasive mini-liposuction under local anesthesia. Most patients report it is well-tolerated. Like any procedure, it carries risks including infection, bleeding, and bruising. Discuss all risks with a physician.
Can anyone bank their adipose tissue? Most healthy adults with enough subcutaneous fat may be candidates. A physician will evaluate appropriateness. Visit the pricing page or contact Save My Fat for details.
Are fat-derived stem cells FDA-approved for any treatment? No. No ADSC-based therapy is FDA-approved. The only FDA-approved stem cell products are hematopoietic progenitor cells from cord blood, approved for specific blood disorders only. The FDA provides patient information about approved products.
How long can banked adipose tissue last? Published studies show meaningful viability after eight or more years of cryopreservation, with some reporting 80 to 91 percent post-thaw viability. Long-term outcomes depend on many factors and cannot be guaranteed. Read the complete banking guide for details.
Can my family members use my banked tissue? First-degree family members may potentially qualify under certain guidelines, though this is not guaranteed. Visit the family page to learn more.
Key Takeaways
Adipose Tissue Is More Than Body Fat
- Fat is a complex organ containing many cell types, including stem cells
- White adipose tissue is the primary source of ADSCs
ADSCs Are Adult Stem Cells, Not Embryonic
- They belong to the mesenchymal stem cell family found in the stromal vascular fraction (SVF)
- Defined by internationally recognized scientific criteria (IFATS/ISCT)
Fat Is One of the Richest Known Sources of MSCs
- Yields roughly 100 to 1,000 times more MSCs per gram than bone marrow
- Collection is minimally invasive
No ADSC-Based Therapy Is FDA-Approved
- The only FDA-approved stem cell products come from cord blood for specific blood disorders
- All other uses are investigational
Research Is Active but Preliminary
- Scientists are studying ADSCs for orthopedic, wound healing, and autoimmune applications
- Being studied does not mean proven safe or effective
Banking Preserves Cells, Not Promises
- Cryopreservation keeps tissue at its current biological age
- Banking does not guarantee access to any treatment, trial, or benefit
Learn More About Adipose Tissue Banking
Understanding the science behind adipose-derived stem cells is an important first step. If preserving your own adipose tissue interests you, the next step is to learn how the process works.
Save My Fat provides adipose tissue banking and cryopreservation services designed to preserve tissue for potential future use in FDA-regulated clinical pathways, not as a treatment or cure for any disease.
To learn more, visit the how stem cell banking works page.
For cost information, visit the pricing page.
Healthcare providers can visit the providers page.
Last updated: March 3, 2026