Patients and providers exploring stem cell banking options will encounter several different tissue sources, from cord blood collected at birth to fat tissue collected at any point in adulthood. Each source has distinct biological characteristics, regulatory classifications, and practical trade-offs. This guide compares birth tissue stem cell sources and adipose-derived stem cells (ADSCs) side by side, covering biology, cell yield, regulatory status, and what the differences mean for tissue banking decisions.
TLDR: Multiple stem cell sources exist. Birth tissue products (cord blood, cord tissue, placenta, amniotic fluid) and adipose tissue each contain different cell types with different biological strengths. Cord blood contains blood-forming stem cells, while cord tissue and adipose tissue contain mesenchymal stem cells (MSCs). Adipose tissue yields far more MSCs per harvest and can be collected at any adult age. Neither source is FDA-approved to treat disease, except five cord blood products approved for specific blood disorders. Understanding these differences helps patients and providers evaluate banking options and future regenerative medicine pathways.
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease. Banking adipose tissue does not guarantee eligibility, access, or clinical benefit from any future therapy, clinical trial, or medical program. All content is for educational purposes only and does not constitute medical advice. Patients must consult their own licensed healthcare professionals regarding all medical decisions.
If you missed the chance to bank cord blood at birth, you might wonder whether the window for stem cell preservation has closed. It has not. Adipose tissue, collected from your own body fat at any point in adulthood, contains large numbers of mesenchymal stem cells that researchers are studying worldwide. This guide uses published, peer-reviewed research to compare these sources so you can make informed decisions.
What Are Birth Tissue Stem Cells?
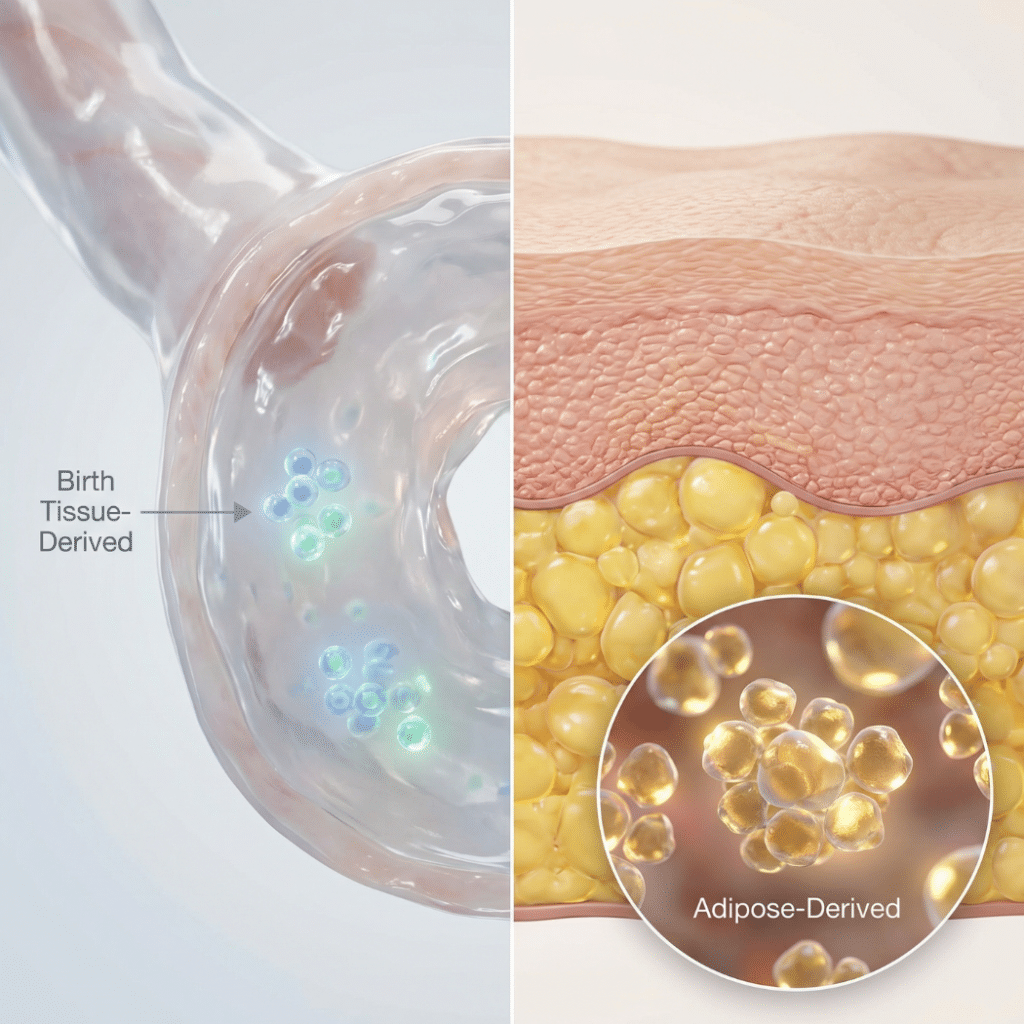
Birth tissue stem cells come from tissues associated with pregnancy and delivery: the umbilical cord, placenta, and amniotic fluid. These tissues are normally discarded after birth, but they contain cells that researchers have found valuable for scientific study.
Types of Birth Tissue Stem Cells
Birth tissue is not a single cell source. It includes several distinct products, each with different cell types:
- Cord blood contains hematopoietic stem cells (HSCs), which are blood-forming cells. These are the basis for the only FDA-approved stem cell products in the United States: five cord blood products (HEMACORD, DUCORD, ALLOCORD, CLEVECORD, and OMISIRGE/omidubicel) licensed for hematopoietic reconstitution in patients with blood disorders. Cord blood also contains a small number of MSCs.
- Cord tissue (specifically Wharton’s jelly, the connective tissue inside the umbilical cord) contains mesenchymal stem cells (WJ-MSCs). These are the birth tissue MSCs most commonly studied in clinical trials. Published research has highlighted their low immunogenicity and secretome profile as areas of scientific interest (Kalaszczynska & Ferdyn, 2015; WJ-MSC secretome review, 2023).
- Placental tissue contains MSCs and other progenitor cells derived from the placenta.
- Amniotic fluid contains amniotic fluid stem cells (AFSCs), a distinct population with some characteristics shared with both MSCs and embryonic stem cells.
Collection Method
All birth tissue is collected at the time of delivery. The process is painless for both mother and child. This is a one-time opportunity; if birth tissue is not collected at delivery, the window is permanently closed.
Birth Tissue Subtypes at a Glance
| Birth Tissue Source | Primary Cell Type | Collection Method | Collection Window |
|---|---|---|---|
| Cord blood | Hematopoietic stem cells (HSCs) | Collected from the umbilical cord vein after delivery | Birth only |
| Cord tissue (Wharton’s jelly) | Mesenchymal stem cells (WJ-MSCs) | Excised section of umbilical cord | Birth only |
| Placental tissue | MSCs, progenitor cells | Collected from the delivered placenta | Birth only |
| Amniotic fluid | Amniotic fluid stem cells (AFSCs) | Amniocentesis or collection during C-section | During pregnancy or at birth |
While cord blood HSC products are FDA-licensed, no cord tissue, placental, or amniotic fluid stem cell product is FDA-approved to treat any disease (FDA patient information on regenerative medicine).
What Are Adipose-Derived Stem Cells?
Adipose-derived stem cells (ADSCs) are mesenchymal stem cells found inside body fat. For a full introduction to ADSC biology, including what the stromal vascular fraction (SVF) is and how ADSCs are identified, see the companion guide: What Are Adipose-Derived Stem Cells?
ADSCs are collected through a minimally invasive mini-liposuction procedure from the abdomen, flanks, or thighs under local anesthesia. The critical difference from birth tissue: adipose tissue can be collected at any point in adulthood. There is no single collection window that closes permanently.
Published research shows that adipose tissue yields approximately 500 to 1,000 times more MSCs per gram than bone marrow, and far more than cord blood. A typical collection of 100 to 200 mL of fat tissue can yield an estimated 50 to 200 million ADSCs, compared to approximately 0.1 to 1 million MSCs from a typical cord blood collection (Kern et al., 2006). ADSCs also demonstrate robust proliferation and multilineage differentiation capacity (Regenerative capacity of ADSCs, MDPI 2019).
For a comparison of ADSCs with bone marrow-derived MSCs specifically, see the companion article: Bone Marrow vs. Adipose-Derived Stem Cells. For details on the banking process, visit the how stem cell banking works page.
Side-by-Side Comparison
This table compares the major stem cell sources across the parameters that matter most for banking and research decisions. All data reflects published, peer-reviewed findings.
| Parameter | Cord Blood | Cord Tissue (WJ-MSCs) | Placental MSCs | Amniotic Fluid (AFSCs) | Adipose (ADSCs) |
|---|---|---|---|---|---|
| Primary cell type | HSCs | MSCs | MSCs | AFSCs | MSCs |
| Collection method | From umbilical cord vein | Cord tissue excision | From delivered placenta | Amniocentesis or C-section | Mini-liposuction (any age) |
| Collection window | Birth only | Birth only | Birth only | Pregnancy/birth | Any time in adulthood |
| Estimated MSC yield | Very low (~0.1-1M MSCs) | Moderate (varies) | Moderate (varies) | Moderate (varies) | Very high (~50-200M MSCs) |
| Isolation success rate | Variable | ~63% | Variable | Variable | ~100% |
| Proliferation capacity | Limited for MSCs | High | High | Very high (250+ doublings reported) | Extensive (50+ doublings) |
| Autologous use | Only for the child | Only for the child | Only for the child | Only for the child | Yes, for the individual |
| Allogeneic use | Yes (with HLA matching) | Yes | Yes | Yes | Possible (with screening) |
| Adipogenic differentiation | N/A (HSCs) | Not observed in some studies | Variable | Variable | Robust, superior |
| Osteogenic differentiation | N/A (HSCs) | Moderate | Moderate | Moderate | Moderate |
| Teratoma risk | None | None | None | None | None |
| FDA-approved products | Yes (5 products for blood disorders) | None | None | None | None |
| Banking availability | At birth only | At birth only | At birth only | During pregnancy | Any adult age |
Sources: Kern et al., 2006; Kalaszczynska & Ferdyn, 2015; Side-by-side MSC comparison, 2013; Wang et al., 2016
This comparison is for educational purposes only. Neither birth tissue MSCs nor ADSCs are FDA-approved to treat any disease (except the five licensed cord blood HSC products for specific blood disorders).
The Telomere Question: Are ADSCs Actually “Younger”?
One of the most common assumptions about stem cells is that “younger” tissue sources automatically produce “younger” cells. Birth tissue is collected from a newborn, so it must contain younger cells than fat tissue from a 40- or 50-year-old adult, right? The published research on this question is more nuanced than most people expect.
What Are Telomeres?
Telomeres are protective caps at the ends of chromosomes, often compared to the plastic tips on shoelaces. Each time a cell divides, its telomeres get slightly shorter. When telomeres become too short, the cell stops dividing and enters senescence (cellular aging). Longer telomeres are generally associated with greater remaining replicative capacity.
What the Research Suggests
Several published studies have explored telomere dynamics in stem cells from different tissue sources. Some key observations from the literature:
ADSCs reside in a quiescent (dormant) state within adipose tissue, nestled within a collagen-rich extracellular matrix that limits active cell division. Because these cells are not regularly cycling, their telomeres may be better preserved than expected based on the donor’s chronological age. This concept, sometimes described as a “protected niche” or dormancy effect, is a theoretical framework discussed in regenerative medicine education. It proposes that the collagen-rich environment of adipose tissue functions as a protective enclosure that shields resident stem cells from the division-related telomere shortening that occurs in more metabolically active tissues.
Published research on telomere biology in stem cell niches has established that tissue-specific environments can influence how quickly stem cells age at the cellular level. Studies by Flores et al. (2008) examined telomerase activity in adult tissue stem cell compartments and found that different niches maintain different levels of telomere protection. Research by Moreno-Navarrete et al. (2010) observed relationships between adipose tissue biology and telomere dynamics that warrant further investigation.
Umbilical cord tissue, while collected at birth, represents tissue at the end of a nine-month developmental lifespan. Wharton’s jelly MSCs have been actively supporting fetal development during that period, meaning some cellular aging and division has already occurred before the tissue is ever banked.
The takeaway for patients: The assumption that birth tissue is always biologically “younger” than adult adipose tissue may be an oversimplification. Published research suggests the relationship between donor age and stem cell quality is more complex than a simple timeline indicates. This area requires more investigation, and neither source should be chosen or dismissed based on age assumptions alone. All claims about telomere preservation in ADSCs remain subjects of active research and are not established scientific consensus.
Autologous vs. Allogeneic: Why the Source Matters
The distinction between autologous (your own cells) and allogeneic (donor cells) is one of the most important practical differences between these stem cell sources.
Birth Tissue Is Allogeneic for Adults
Birth tissue stem cells are collected from the baby’s umbilical cord, placenta, or amniotic fluid. This means they are autologous only for the child from whom they were collected. For any other person, including the child’s parents, siblings, or any other family member, birth tissue stem cells are allogeneic (from a donor).
Allogeneic cell use requires consideration of HLA matching (human leukocyte antigen matching), which determines how well the immune system will tolerate foreign cells. Mismatched allogeneic cells carry risks of immune rejection and, in some cases, graft-versus-host disease (GVHD). WJ-MSCs do show lower immunogenicity than many other allogeneic sources in published studies, which is one reason researchers are interested in them (Wang et al., 2016).
Adipose Tissue Is Autologous for the Banking Individual
ADSCs collected from a person’s own fat tissue are inherently autologous. There is no HLA matching concern and no immune rejection risk when cells are used by the same individual. First-degree family members may also potentially qualify to use banked cells under certain guidelines. Visit the family page for more information.
FDA Regulatory Classification
How the FDA classifies a stem cell product depends on how the tissue is processed and what claims are made about its intended use. Both birth tissue and adipose tissue fall under 21 CFR Part 1271, the FDA’s framework for human cells, tissues, and cellular and tissue-based products (HCT/Ps).
Birth Tissue Products
The five FDA-licensed cord blood products went through the full Section 351 Biologics License Application (BLA) pathway. They are approved exclusively for hematopoietic reconstitution in patients with specific blood disorders. No cord tissue, placental, or amniotic stem cell product is FDA-approved to treat any disease.
Many birth tissue products marketed commercially as “stem cell treatments” or “regenerative therapies” have not gone through FDA approval. The FDA has issued guidance about how HCT/P products are classified and regulated.
Adipose Tissue Products
Adipose tissue that is minimally manipulated (such as microfragmented adipose tissue, or MFAT) and used homologously may qualify under the Section 361 HCT/P pathway. Adipose tissue that undergoes enzymatic digestion to isolate SVF, or culture expansion to isolate ADSCs, is generally classified as more than minimally manipulated. This places those products under the Section 351 pathway, requiring IND/BLA and FDA approval before marketing.
Neither birth tissue MSC products nor adipose-derived SVF/ADSCs are FDA-approved to treat any disease. The only exception is the five licensed cord blood products for blood disorders. Patients should always verify FDA approval status before pursuing any product marketed as a stem cell treatment.
Clinical Trial Landscape
Both birth tissue stem cells and adipose-derived stem cells are subjects of active clinical research worldwide. Registered clinical trials can be found on ClinicalTrials.gov.
Published data shows MSC source distribution in orthopedic trials breaks down approximately as: bone marrow (26.5%), adipose tissue (20.5%), and umbilical cord (15.4%), with other sources making up the remainder. ADSCs represent the second most common MSC source in registered trials.
Perinatal MSC trials (particularly WJ-MSCs) are growing in number, with research focused on neurological conditions, graft-versus-host disease, and cerebral palsy. The CERES trial (NCT03059355) is one example of a head-to-head comparison design between umbilical cord MSCs and bone marrow MSCs.
For more on areas where researchers are studying ADSCs, visit the emerging research page and the pages on joint and orthopedic research and wellness and healthy aging.
Clinical trials are research studies, not treatment programs. Being listed on ClinicalTrials.gov does not mean a product is proven safe, effective, or FDA-approved. Participation is voluntary and subject to strict eligibility criteria. Results are not guaranteed.
Practical Considerations for Banking
When it comes to preserving stem cells for potential future use, the practical differences between these sources are significant.
Birth Tissue Banking
The decision to bank cord blood or cord tissue must be made before or during delivery. If birth tissue was not collected at birth, the window is permanently closed. For parents who did not bank (or whose children are already grown), this option is no longer available.
Adipose Tissue Banking
Adipose tissue can be collected at any point in adulthood when the patient is healthy enough to undergo a minimally invasive liposuction procedure. There is no single deadline that closes permanently. A single harvest yields far more MSCs than a typical cord blood collection, and the cells are autologous (the patient’s own).
Save My Fat provides adipose tissue banking as a preservation service. The tissue is cryopreserved at the patient’s current biological age for potential future use in FDA-regulated clinical pathways. Banking does not guarantee access to any treatment, clinical trial, or medical program. For information on cost, visit the pricing page.
What Questions Should You Ask Your Provider?
Before making any decision about stem cell banking, patients should bring these questions to their healthcare provider:
- Is the product being offered FDA-approved for the claimed use?
- What published evidence supports the claims being made?
- What are the potential risks, and what is the realistic range of outcomes?
- Does the company have any FDA warning letters or enforcement actions?
- How are the cells processed, and does that processing change the regulatory classification?
- What is the long-term viability data for cryopreserved tissue from this source?
- What is the difference between autologous and allogeneic use, and which applies to my situation?
Asking these questions helps distinguish between legitimate preservation services and clinics marketing unapproved products. Learn more on the Save My Fat about page or the providers page.
Frequently Asked Questions
What are birth tissue stem cells, and where do they come from? Birth tissue stem cells come from tissues associated with pregnancy and delivery, including umbilical cord blood (which contains blood-forming HSCs), cord tissue or Wharton’s jelly (which contains MSCs), the placenta, and amniotic fluid. These are collected at the time of birth and are the baby’s cells, not the mother’s.
Which source produces more stem cells per harvest? Adipose tissue yields significantly more MSCs per harvest than any birth tissue source. A typical fat collection yields an estimated 50 to 200 million MSCs, compared to approximately 0.1 to 1 million from cord blood (Kern et al., 2006). ADSCs also proliferate faster and retain multipotency through more culture passages in published studies (Mohamed-Ahmed et al., 2018).
Are birth tissue stem cells “younger” than adipose-derived stem cells? Not necessarily. While birth tissue is collected at delivery, published research suggests that ADSCs reside in a quiescent niche that may preserve their biological characteristics. The relationship between donor age and stem cell quality is more complex than simple chronological age. More research is needed.
Can I bank my own adipose tissue as an adult? Yes. Unlike birth tissue, which can only be collected at the time of delivery, adipose tissue can be collected through a mini-liposuction at any point in adulthood. This is one of the primary practical advantages of adipose tissue banking.
What is the difference between autologous and allogeneic? Autologous means the cells come from your own body. Allogeneic means they come from a donor. ADSCs from your own fat are autologous. Birth tissue is autologous only for the child from whom it was collected; for everyone else, it is allogeneic.
Are either of these stem cell sources FDA-approved to treat diseases? Five cord blood HSC products are FDA-licensed for hematopoietic reconstitution in patients with specific blood disorders. No cord tissue, placental, amniotic fluid, or adipose-derived stem cell product is FDA-approved to treat any disease. The FDA provides patient information about approved products.
Why does Save My Fat focus on adipose tissue? Adipose tissue offers practical advantages for banking: significantly higher MSC yield, a less invasive collection procedure, the ability to collect at any adult age, and autologous use. For patients who did not bank birth tissue or whose children are already grown, adipose tissue represents an accessible alternative.
Are there clinical trials comparing birth tissue and adipose stem cells? Yes. Clinical trials registered on ClinicalTrials.gov include studies investigating both adipose-derived and perinatal MSCs for various research applications. Head-to-head comparison designs do exist, though most trials study one source at a time. All trials are research, not treatment.
What is the difference between cord blood banking and adipose tissue banking? Cord blood banking preserves blood-forming stem cells (HSCs) collected at birth for potential use in blood disorder treatments. Adipose tissue banking preserves MSCs collected from adult fat tissue for potential future use in FDA-regulated clinical pathways. They preserve different cell types from different tissue sources at different points in life.
Do commercially marketed birth tissue products always contain viable stem cells? Published research has raised questions about how many viable stem cells survive the processing, freezing, and thawing of certain commercial birth tissue products. Patients should ask for viability data and verify all claims with the FDA consumer alert on regenerative medicine products.
Key Takeaways
Both Sources Contain Valuable Cells, But They Are Not Identical
- Cord blood primarily contains blood-forming HSCs; cord tissue and adipose tissue contain MSCs
- These are different stem cell types with different biological functions and research applications
Adipose Tissue Offers a Major Yield Advantage
- A single fat collection yields an estimated 50 to 200 million MSCs
- Cord blood yields approximately 0.1 to 1 million MSCs per collection
Collection Timing Is a Critical Differentiator
- Birth tissue can only be collected at the time of delivery; the window closes permanently
- Adipose tissue can be collected at any point in healthy adulthood
Autologous vs. Allogeneic Matters
- ADSCs from your own fat are autologous (no immune rejection concern)
- Birth tissue is allogeneic for anyone except the child from whom it was collected
Neither Source Is FDA-Approved to Treat Disease (With One Exception)
- Five cord blood HSC products are FDA-licensed for specific blood disorders only
- No cord tissue, placental, amniotic, or adipose MSC product is FDA-approved for disease treatment
The “Younger Is Always Better” Assumption May Be an Oversimplification
- Published research suggests ADSCs may maintain biological characteristics due to their quiescent niche environment
- More research is needed on telomere dynamics across tissue sources and donor ages
Learn More About Adipose Tissue Banking
Before contacting Save My Fat: Adipose tissue banking is a preservation service for potential future opportunities, not a treatment or cure for any disease. Outcomes cannot be guaranteed. All medical decisions must be made with a licensed healthcare provider.
Save My Fat provides adipose tissue banking and cryopreservation services designed to preserve tissue for potential future use in FDA-regulated clinical pathways.
Visit the how stem cell banking works page to learn about the process.
For cost information, visit the pricing page.
Healthcare providers can visit the providers page or the stem cell research areas page for clinical context.
Last updated: March 6, 2026