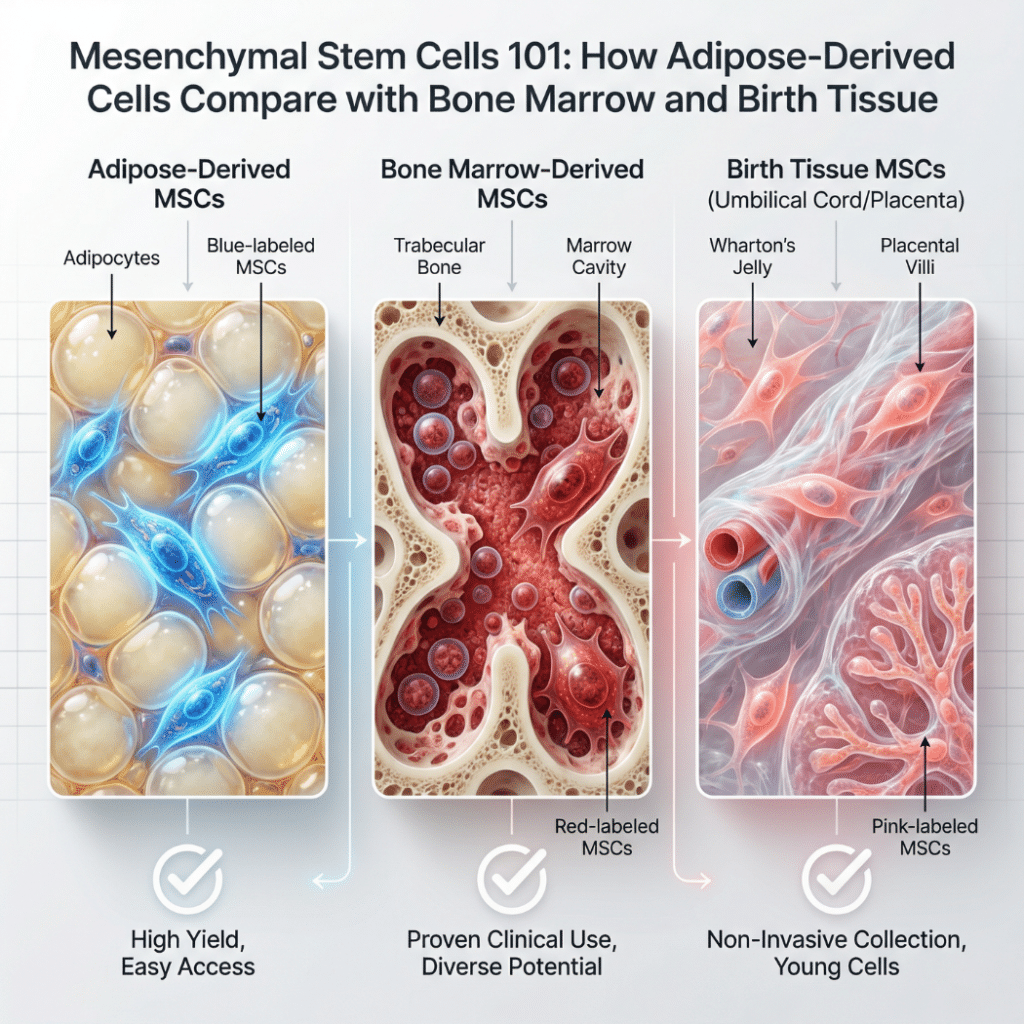
Mesenchymal stem cells, often abbreviated MSCs, are a family of multipotent cells found in bone marrow, adipose (fat) tissue, umbilical cord, and other tissues throughout the body. These cells can differentiate into bone, cartilage, and fat under laboratory conditions and are being studied in hundreds of clinical trials for their regenerative and immunomodulatory properties. Each tissue source offers distinct advantages and tradeoffs that shape how researchers approach different applications.
TLDR: MSCs are defined in the lab by three criteria: they grow on plastic, they express specific surface markers (CD73, CD90, CD105 positive; blood cell markers negative), and they can become bone, cartilage, and fat cells in culture. Adipose tissue, bone marrow, and birth tissue MSCs share these core features but differ in yield, proliferation rate, and functional properties. No single source has proven best for all applications, which is why researchers continue to compare them. Read on for a complete breakdown of MSC biology and what source differences mean for patients.
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease. Banking adipose tissue does not guarantee eligibility, access, or clinical benefit from any future therapy, clinical trial, or medical program. All content below is for educational purposes only and does not constitute medical advice. Patients must consult their own licensed healthcare professionals regarding all medical decisions.
If you have been reading about regenerative medicine, you have almost certainly encountered the term “mesenchymal stem cell.” It appears in clinical trial listings, research news, and marketing from clinics worldwide. But the term can be confusing, especially when different sources use different names for what appears to be the same cell type.
The confusion matters because MSC science sits at the center of a rapidly growing field. Hundreds of clinical trials are investigating MSCs for conditions from osteoarthritis to graft-versus-host disease. At the same time, unregulated clinics have used the “stem cell” label to market unapproved treatments, making it harder for patients to distinguish evidence from hype.
This guide breaks down what MSCs are, how scientists define them, what they actually do, and how MSCs from adipose tissue compare with those from bone marrow and birth tissues. You will learn why surface markers matter, why the naming debate is more than semantics, and how source differences influence research design.
What Are Mesenchymal Stem Cells?
MSCs are multipotent stromal cells that can give rise to several cell types of mesodermal origin, including osteoblasts (bone-forming cells), chondrocytes (cartilage cells), and adipocytes (fat cells). This capacity to differentiate into multiple lineages distinguishes them from pluripotent embryonic stem cells, which can become virtually any cell type.
The cells were first observed in 1970 by Alexander Friedenstein in bone marrow and later named “mesenchymal stem cells” by Arnold Caplan in 1991. The name has been debated ever since. The International Society for Cellular Therapy (ISCT) recommends using “mesenchymal stromal cells” because true stem cell behavior has not been conclusively demonstrated for all MSC preparations (Viswanathan et al., 2019). Caplan himself proposed renaming them “Medicinal Signaling Cells” in 2017, arguing their primary function is paracrine signaling rather than direct tissue replacement (Caplan, 2017). In practice, all three terms refer to largely the same cell populations, and the abbreviation “MSC” is used across research regardless of preferred full name.
MSCs are being studied in a wide range of conditions for their immunomodulatory and trophic effects, but evidence of clinical effectiveness is still developing for most indications. The vast majority of MSC applications remain investigational.
How Scientists Define an MSC: The ISCT Minimal Criteria
In 2006, the ISCT published a position statement establishing three minimum criteria for classifying cells as multipotent mesenchymal stromal cells (Dominici et al., 2006). This paper has been cited over 15,000 times and remains the global standard.
| Criterion | Requirement | Details |
|---|---|---|
| Plastic adherence | Cells must adhere to standard tissue culture plastic | When maintained in standard culture conditions, MSCs attach and grow on plastic surfaces |
| Surface marker profile | Specific positive and negative markers | At least 95% of cells must express CD105, CD73, and CD90; no more than 2% may express CD45, CD34, CD14/CD11b, CD79a/CD19, or HLA-DR |
| Trilineage differentiation | Differentiation into three mesodermal lineages | Under appropriate in vitro conditions, cells must form osteoblasts (bone), adipocytes (fat), and chondroblasts (cartilage) |
These criteria were intentionally set as a minimum floor. Many researchers use additional markers such as CD44, CD146, STRO-1, CD29, and CD166 to further characterize preparations, but these are not part of the formal definition. Surface markers alone do not prove that a cell population will behave as a stem cell or produce a therapeutic effect.
What MSCs Actually Do: Differentiation, Paracrine Signaling, and Immunomodulation
Early models of MSC therapy assumed MSCs would engraft and differentiate into replacement cells. Current evidence tells a more nuanced story. While MSCs can differentiate into bone, cartilage, and fat under lab conditions, their most important functions in a living organism appear to be paracrine signaling and immunomodulation (Pittenger et al., 2019).
| Function | Mechanism | Key Details |
|---|---|---|
| Differentiation | Direct cell replacement | MSCs can form osteoblasts, chondrocytes, and adipocytes in culture; broader in vivo potential remains controversial |
| Paracrine signaling | Secretion of bioactive molecules | MSCs release cytokines (cell communication molecules), chemokines, growth factors, and extracellular vesicles (tiny cell-released packages) that influence tissue repair and blood vessel formation |
| Immunomodulation | Interaction with immune cells | MSCs interact with T cells, B cells, NK cells, macrophages, and dendritic cells to dampen excessive inflammation and support immune balance |
For patients, the key point is this: when you read about MSC research, the cells are most likely being studied for their ability to modulate inflammation and support the body’s own repair processes, not simply for their ability to “turn into” new tissue. This distinction shapes how clinical trials are designed and what outcomes researchers measure.
Three Major Sources: Adipose, Bone Marrow, and Birth Tissue
Three sources dominate MSC research and clinical development. Each produces cells that meet the ISCT criteria but differ in meaningful ways. For broader context, see the Save My Fat pages on adipose-derived stem cells and emerging research.
| Feature | Adipose Tissue MSCs | Bone Marrow MSCs | Birth Tissue MSCs (Cord, Wharton’s Jelly, Placenta) |
|---|---|---|---|
| Source type | Adult tissue (subcutaneous fat) | Adult tissue (bone marrow) | Neonatal tissues collected after delivery |
| Collection | Mini-liposuction or surgical fat harvest | Bone marrow aspiration; more invasive | Post-delivery collection; no risk to mother or infant |
| MSC yield | High: ~350,000 to 1,000,000 cells per gram | Low: ~500 to 50,000 cells per gram | Variable; cord tissue shows good expansion potential |
| Differentiation biases | Strongest adipogenic capacity; robust osteogenic and chondrogenic potential | Often stronger osteogenic potential | High proliferation; differentiation patterns vary by compartment |
| Immunomodulation | Potent paracrine and anti-inflammatory effects | Well-studied immunomodulatory effects | Low immunogenicity with strong paracrine activity; attractive for allogeneic use |
| Clinical trial experience | Numerous early-phase trials in orthopedic, vascular, and autoimmune indications | Longest track record; hundreds of trials | Growing trial numbers in neurological and inflammatory conditions |
This table describes research use, not approved treatments. No MSC source has been proven superior across all conditions.
Adipose-Derived MSCs: What Makes Them Distinct
Adipose tissue was first identified as an MSC source by Zuk and colleagues in 2001, who demonstrated that lipoaspirate cells could differentiate into multiple lineages (Zuk et al., 2001). The most notable advantage is yield: one gram of adipose tissue produces roughly 100 to 500 times more MSCs than an equivalent amount of bone marrow (Bourin et al., 2013).
| Characteristic | Finding | Reference |
|---|---|---|
| Yield per gram | 350,000 to 1,000,000 cells | Bourin et al., 2013 (IFATS/ISCT) |
| Core ISCT markers | CD73+, CD90+, CD105+; CD45-, CD34- after culture | Bourin et al., 2013 |
| Distinguishing marker | CD36+ (vs. bone marrow) | IFATS/ISCT joint statement |
| Adipogenic differentiation | Strongest among three major sources | Kern et al., 2006 |
| Proliferation rate | Faster than bone marrow MSCs | Multiple comparative studies |
AD-MSCs are being studied in trials for osteoarthritis, critical limb ischemia, autoimmune diseases, and other conditions. These remain investigational. For deeper exploration of adipose tissue biology and the stromal vascular fraction, see the related guides. To understand how adipose tissue banking preserves tissue containing MSCs alongside other supportive cells and matrix, visit the complete banking guide.
Bone Marrow MSCs: The Original Standard
Bone marrow was the first source from which MSCs were rigorously defined. BM-MSCs often demonstrate stronger osteogenic differentiation compared with adipose-derived MSCs, making them a natural focus for bone and orthopedic research. However, practical limitations are significant. MSC frequency in bone marrow is low (0.001% to 0.01% of nucleated cells), aspiration is more invasive than liposuction, and both yield and proliferative capacity decline with donor age.
| Age-Related Change | Finding | Reference |
|---|---|---|
| Senescence markers | 4-fold increase in older vs. younger donors | Zhou et al., 2008 |
| Doubling time | 1.7-fold longer with advancing age | Zhou et al., 2008 |
| Colony frequency | Significant decline in CFU-F with age | Stolzing et al., 2008 |
For a detailed comparison, see the bone marrow vs. adipose stem cells guide. Despite these limitations, BM-MSCs carry the longest clinical track record and many early safety datasets were based on bone marrow-derived products.
Birth Tissue MSCs: Umbilical Cord and Placenta
Umbilical cord, Wharton’s jelly, and placenta are neonatal tissues that would otherwise be discarded after delivery. They produce MSCs with high proliferative capacity and low immunogenicity, properties attractive for allogeneic (donor-to-patient) applications (Jin et al., 2013). Some birth tissue MSCs express HLA-G, an immunomodulatory molecule that helps the placenta avoid immune rejection and may contribute to low immunogenicity.
However, birth tissue MSCs raise distinct considerations. They are typically used as allogeneic products, adding manufacturing and regulatory complexity. In Kern and colleagues’ comparative study, cord blood MSCs could not differentiate into adipocytes where bone marrow and adipose MSCs readily did, suggesting source tissue shapes differentiation capacity in application-relevant ways (Kern et al., 2006). For more, see the birth tissue vs. adipose stem cells guide.
MSC Surface Markers and the Problem of Heterogeneity
The ISCT panel (CD73, CD90, CD105 positive; CD45, CD34, CD14, CD79a, HLA-DR negative) is necessary but not sufficient for identifying functionally competent MSC populations (Lv et al., 2014).
| Marker Category | Examples | Significance |
|---|---|---|
| ISCT core positive | CD73, CD90, CD105 | Required; expressed by at least 95% of cells |
| ISCT core negative | CD45, CD34, CD14/CD11b, CD79a/CD19, HLA-DR | Must be absent (less than 2%); rules out blood cell contamination |
| Common additional markers | CD44, CD29, CD166 | Broadly expressed across MSC preparations from all sources |
| Stemness-associated markers | STRO-1, CD146, CD271, SSEA-4 | May enrich for more potent subpopulations; expression varies by source |
| Source-distinguishing markers | CD36 (adipose), CD106 (bone marrow), Oct-4 (some birth tissue) | Help distinguish MSCs from different tissue origins |
A critical insight is “phenotypic convergence”: standard culture causes many cell types to acquire MSC-like marker profiles over successive passages. Two preparations can look identical by flow cytometry yet behave very differently in functional assays. Potency assays and functional characterization are increasingly recognized as essential supplements to marker analysis.
How Source Differences Might Matter in Research
Source tissue influences MSC behavior across several dimensions relevant to clinical translation. These differences help explain why researchers studying stem cell research areas may select different MSC sources for different conditions.
| Research Dimension | How Source Matters |
|---|---|
| Gene expression | Baseline transcriptomes differ between AD-MSCs, BM-MSCs, and UC-MSCs, reflecting tissue of origin |
| Differentiation biases | BM-MSCs tend toward stronger osteogenesis; AD-MSCs toward stronger adipogenesis; UC-MSCs show high proliferation but variable differentiation |
| Senescence and aging | UC-MSCs show lowest senescence; BM-MSCs show most age-related decline; AD-MSC yield is less affected by donor age |
| Secretome composition | Cytokine and growth factor profiles differ by source, potentially influencing application suitability |
No single source is universally superior. The December 2024 FDA approval of Ryoncil (remestemcel-L), the first MSC product approved in the United States, used bone marrow-derived MSCs for pediatric steroid-refractory acute graft-versus-host disease (FDA, 2024). This milestone demonstrates that a rigorous regulatory pathway can work for MSC products, but it applies to one product, one indication, and one source.
Adipose tissue banking preserves a rich stromal compartment containing MSCs alongside other supportive cells and extracellular matrix. Any future use in FDA-regulated pathways would depend on specific products, protocols, and trials, and cannot be promised today. To learn how the banking process works, visit the process page.
Frequently Asked Questions
Are mesenchymal stem cells and mesenchymal stromal cells the same thing?
They refer to largely the same cell populations. The ISCT recommends “stromal cells” because not all preparations meet strict stem cell criteria. Caplan later proposed “Medicinal Signaling Cells.” In practice, the abbreviation MSC is used regardless of preferred full name.
How do scientists confirm a culture contains MSCs?
By applying the ISCT minimal criteria: plastic adherence, expression of CD105, CD73, and CD90 (while lacking CD45, CD34, and other blood cell markers), and differentiation into bone, fat, and cartilage cells. Many groups add functional assays because meeting these criteria alone does not guarantee therapeutic potency.
What is the difference between adipose-derived MSCs and bone marrow MSCs?
Both meet ISCT criteria, but adipose provides 100 to 500 times more MSCs per gram, with faster proliferation. Bone marrow MSCs tend toward stronger bone formation. Some secondary markers differ, including CD36 (adipose) and CD106 (bone marrow). For a full comparison, see the bone marrow vs. adipose stem cells guide.
Are birth tissue MSCs stronger or safer than adult tissue MSCs?
Birth tissue MSCs proliferate faster and show lower immunogenicity, making them attractive for allogeneic use. However, “stronger” depends on the application. They may not differentiate as readily into certain cell types. Safety profiles for all three sources appear favorable in early data, but long-term comparative studies are limited.
What do markers like CD73, CD90, and CD105 mean?
These are surface proteins detected by flow cytometry. CD73 is an enzyme involved in signaling, CD90 is a glycoprotein associated with cell adhesion, and CD105 (endoglin) participates in cell signaling pathways. Their presence on at least 95% of cells, combined with absent blood cell markers, is one of three ISCT classification criteria.
Do MSCs work mainly by becoming new tissue or by signaling other cells?
Current evidence strongly supports paracrine signaling as the primary mechanism. MSCs secrete cytokines, growth factors, and extracellular vesicles that modulate immune responses and support endogenous repair, rather than persisting long-term as replacement tissue.
Are all MSC therapies approved by the FDA?
No. As of early 2025, the FDA has approved one MSC product: Ryoncil for pediatric steroid-refractory acute graft-versus-host disease. Most MSC applications remain investigational. Patients should be cautious about clinics marketing unapproved MSC “treatments.” See the guide on banking vs. stem cell treatment clinics for more.
Why do experts argue about what to call these cells?
The name shapes patient expectations. “Stem cell” implies robust regenerative capacity not conclusively demonstrated in vivo. “Stromal cells” sets more accurate expectations. “Medicinal Signaling Cells” emphasizes signaling functions. Despite these proposals, “mesenchymal stem cells” remains the most widely used term.
Can banking my fat guarantee I will receive an MSC treatment?
No. Banking preserves tissue containing MSCs, but it does not guarantee eligibility for any trial, Expanded Access program, or future therapy. Any future use depends on regulatory status, clinical situation, physician guidance, and availability of FDA-regulated pathways. Save My Fat does not provide treatments or therapies.
How can I find legitimate MSC clinical trials?
Search ClinicalTrials.gov by condition and terms like “mesenchymal stem cells” or “adipose.” Look for registered NCT numbers, verify recruiting status, and discuss any trial with your physician before contacting the study team. For a walkthrough, see the guide to finding legitimate clinical trials.
Key Takeaways
MSC Definition and Biology
- MSCs are defined by three ISCT criteria: plastic adherence, a specific surface marker profile, and trilineage differentiation
- Paracrine signaling and immunomodulation, not direct tissue replacement, are the primary mechanisms in most therapeutic contexts
- The naming debate reflects real scientific uncertainty about in vivo stem cell behavior
Source Comparison
- Adipose tissue provides the highest MSC yield (100 to 500 times more than bone marrow) with simpler collection
- Bone marrow MSCs carry the longest clinical track record and often show stronger osteogenic potential
- Birth tissue MSCs offer high proliferation and low immunogenicity for potential allogeneic use
- No single source is universally superior; the best choice depends on the application under investigation
Surface Markers and Heterogeneity
- The ISCT panel is a minimum standard, not a complete characterization
- Culture expansion causes phenotypic convergence, making functional assays essential
- Source-specific marker differences (CD36, CD106, HLA-G) help distinguish MSC origins
Clinical Landscape
- Over 1,500 MSC trials are registered worldwide, most in early phases
- The FDA approved its first MSC product (Ryoncil) in December 2024 for one specific indication
- Patients should be skeptical of clinics marketing unapproved MSC treatments for diseases
Disclaimer: This article is for educational purposes only and does not provide medical advice or recommend specific therapies. Mesenchymal cell-based interventions discussed here are largely investigational and should only be accessed through regulated pathways such as clinical trials or appropriately authorized programs. Save My Fat does not provide treatments, run trials, or enroll patients in investigational programs. Banking tissue does not guarantee access to future therapies or clinical benefit. All medical decisions should be discussed with licensed healthcare professionals.
Learn More
Before contacting Save My Fat: Adipose tissue banking is a preservation service for potential future opportunities, not a treatment or cure for any disease. Outcomes cannot be guaranteed. All medical decisions must be made with a licensed healthcare provider.
To explore adipose tissue and MSC science further, visit the Save My Fat pages on adipose-derived stem cells, adipose tissue biology, and emerging research.
To understand the banking process, visit how stem cell banking works.
Healthcare providers can learn more on the providers page.
Patients curious about MSC research should discuss options with their own clinicians and review registered studies at ClinicalTrials.gov.
Last updated: March 17, 2026







