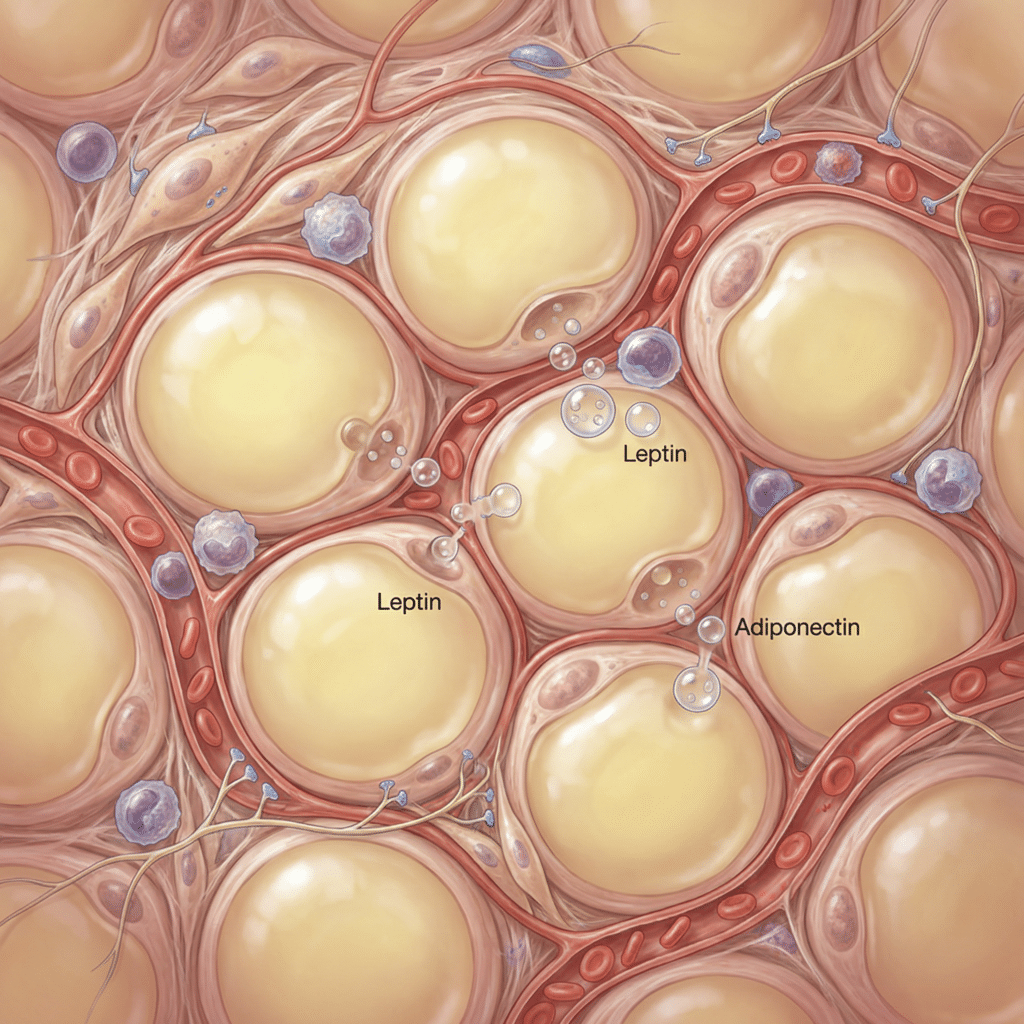
For most of the 20th century, scientists treated body fat as biological packing material: a passive depot that stored calories and cushioned organs. That view changed dramatically in 1994 when researchers discovered leptin, a hormone produced almost exclusively by fat cells. That single finding proved that adipose tissue actively communicates with the brain to regulate appetite and energy balance. In the decades since, researchers have identified dozens of additional signaling molecules secreted by fat, and modern science now recognizes adipose tissue as one of the largest endocrine organs in the human body.
This guide explains what adipose tissue actually does, how its health changes with age and metabolism, what cell populations live inside it, and why these biological properties are relevant to people considering adipose tissue banking. You will come away with a clearer understanding of why fat is far more than you think, and why the state of your adipose tissue at the time of banking matters from a biological standpoint.
TLDR: Adipose tissue is not inert storage. It is an active endocrine organ that secretes signaling molecules called adipokines, including leptin, adiponectin, and several inflammatory cytokines, that influence appetite, insulin sensitivity, cardiovascular health, and immune function. Different fat depots (subcutaneous vs. visceral) behave differently and carry different metabolic risk profiles. Adipose tissue also contains a rich population of mesenchymal stromal cells and other supporting cells that are the subject of hundreds of ongoing clinical research studies. The biological state of adipose tissue at the time of collection may influence cell yields and laboratory measures such as viability, but this does not translate directly into guaranteed clinical benefit for any individual. Banking preserves options, not outcomes.
Important Disclaimer: Save My Fat does not provide FDA-approved treatments or cures for any disease. Banking adipose tissue does not guarantee eligibility, access, or clinical benefit from any future therapy, clinical trial, or medical program. All content is for educational purposes only and does not constitute medical advice. Patients must consult their own licensed healthcare professionals regarding all medical decisions.
From “Storage” to Endocrine Organ
The discovery of leptin at Rockefeller University in 1994 was a turning point. It demonstrated that fat cells do not simply sit quietly waiting to release stored energy. They actively produce hormones that travel through the bloodstream and influence distant organs. Since then, researchers have identified dozens of signaling molecules secreted by adipose tissue, collectively called adipokines. These molecules influence metabolism, insulin sensitivity, cardiovascular health, immune function, brain function, and reproduction (Ronti et al., 2006; Scherer, 2006).
Think of adipose tissue as a broadcasting station. Every day, your fat is sending chemical messages to your brain (“here is how much energy we have stored”), your pancreas (“adjust insulin production”), your heart and blood vessels (“here are signals affecting clot risk and vessel inflammation”), and your immune system (“here is the current inflammatory state”). When adipose tissue is healthy, these messages are balanced. When it is dysfunctional, due to excess visceral fat, chronic inflammation, or metabolic disease, the signals become distorted, contributing to conditions like insulin resistance and cardiovascular disease.
Modern science now classifies adipose tissue as one of the largest endocrine organs in the body. It is an active participant in nearly every major physiological system (Endotext, 2020).
What Your Fat Is Actually Doing Day to Day
The specific adipokines that adipose tissue produces, and in what quantities, determine much of its impact on your health. Here are the major players:
| Adipokine | Produced By | Main Roles | Clinical Relevance |
|---|---|---|---|
| Leptin | White adipocytes (proportional to fat mass) | Appetite regulation, energy balance, reproductive function, immune signaling | Leptin resistance is a hallmark of obesity; elevated levels associated with cardiovascular risk |
| Adiponectin | White adipocytes (inversely proportional to fat mass) | Insulin sensitization, anti-inflammatory effects, cardioprotection, fatty acid oxidation | Low levels associated with metabolic syndrome, type 2 diabetes, cardiovascular disease |
| Resistin | White adipocytes and immune cells | Implicated in insulin resistance (role in humans less clear than in rodent models) | Elevated in inflammatory conditions |
| TNF-alpha | Adipose tissue macrophages | Pro-inflammatory cytokine; contributes to insulin resistance | Elevated in obesity; linked to chronic low-grade inflammation |
| IL-6 | Adipocytes and supporting cell populations | Dual role: pro-inflammatory systemically, may have local anti-inflammatory effects | Elevated in visceral obesity; linked to cardiovascular risk |
| Estrogen | Adipose tissue aromatase enzyme | Converts androgens to estrogen | Relevant in post-menopausal health and hormone-sensitive conditions |
| PAI-1 | Adipocytes | Inhibits blood clot breakdown (fibrinolysis) | Elevated in obesity; contributes to thrombotic risk |
Sources: Ronti et al., 2006; Endotext, 2020
The balance between these signals matters. Adiponectin, for example, is protective: it helps cells respond to insulin and reduces inflammation. But adiponectin levels drop as fat mass increases, especially visceral fat. Meanwhile, TNF-alpha, IL-6, and PAI-1 tend to rise with excess fat, pushing the body toward a state of chronic, low-grade inflammation that underlies many metabolic diseases.
This is not a simple “fat is bad” story. Adipose tissue in a healthy state produces a balanced profile of signals that support normal metabolism. The problems emerge when that balance shifts, often due to excess visceral fat, sedentary behavior, or metabolic disease.
Subcutaneous vs. Visceral Fat: Why Location Matters
Not all fat behaves the same way. Where fat is located in the body has a significant impact on its metabolic behavior and health implications.
Subcutaneous fat sits beneath the skin, primarily around the abdomen, thighs, hips, and arms. Visceral fat wraps around internal organs in the abdominal cavity, including the omentum and mesentery. They look similar on imaging, but their biology is quite different.
| Parameter | Subcutaneous Fat (SAT) | Visceral Fat (VAT) |
|---|---|---|
| Location | Beneath the skin (abdomen, thighs, hips, arms) | Around internal organs (omentum, mesentery) |
| Proportion of total body fat | ~80% in lean individuals | ~10-20% in lean individuals |
| Adipokine profile | Higher adiponectin (anti-inflammatory) | Higher pro-inflammatory cytokines (IL-6, TNF-alpha) |
| Metabolic risk per volume | Lower | Strongly associated with insulin resistance, cardiovascular disease, type 2 diabetes |
| Mesenchymal stromal cell yield | High (2-5 x 10^5 cells per mL from abdominal depot) | Lower yield; more inflammatory cell infiltration |
| Used for tissue banking | Yes (primary harvest site) | Not typically harvested |
Sources: Endotext, 2020; MDPI, 2025
The fat under your skin, particularly from the abdomen and flanks, is the type harvested for adipose tissue banking. It is metabolically different from the deep visceral fat around your organs, and it is also where the highest concentration of adipose-derived mesenchymal stromal cells resides. This is not a coincidence. Subcutaneous depots tend to have a more favorable cellular composition for preservation and research purposes.
The Cellular Ecosystem Inside Adipose Tissue
Fat cells (adipocytes) make up the majority of adipose tissue by volume, but they are not the majority by cell count. The non-fat cell populations inside adipose tissue form a diverse biological ecosystem that includes mesenchymal stromal cells (approximately 15 to 30% of the non-fat cell population), endothelial cells that line blood vessels (10 to 20%), pericytes that support vessel walls (3 to 5%), and various immune cells including macrophages, granulocytes, and lymphocytes (Bourin et al., 2013).
The mesenchymal stromal cells within this ecosystem are identified by internationally agreed criteria established by IFATS and ISCT. The cells must adhere to plastic surfaces in culture, express specific surface markers (CD73, CD90, CD105) while lacking others (CD14, CD34, CD45, HLA-DR), and demonstrate the ability to differentiate into fat, bone, and cartilage cells under laboratory conditions.
What makes these cells particularly interesting to researchers is their secretome: the collection of bioactive molecules they release into their environment. Published research has identified over 80 secreted factors from adipose-derived mesenchymal stromal cells, including vascular endothelial growth factor (VEGF), hepatocyte growth factor (HGF), and multiple anti-inflammatory mediators. The cells also produce extracellular vesicles that carry proteins, lipids, and nucleic acids as a form of cell-to-cell communication.
Current research indicates that these cells act primarily through paracrine signaling (releasing helpful molecules into their surroundings) rather than engrafting and replacing damaged tissue directly. This means the research interest is largely about what these cells release, not just whether they survive at a target site. This research is ongoing, investigational, and has not produced any FDA-approved products for disease treatment as of March 2026.
How Adipose Tissue Health Changes with Age and Metabolism
Adipose tissue biology does not remain constant throughout life. Published research has documented several age-related changes that affect both metabolic function and the tissue’s cellular properties.
One of the most visible changes is fat redistribution. Subcutaneous fat tends to decrease while visceral fat increases with age, shifting the body’s adipose profile toward a more inflammatory state. At the cellular level, aging is associated with chronic low-grade inflammation (sometimes called “inflammaging”), accumulation of senescent cells that no longer divide but release inflammatory signals, declining brown and beige fat activity, increased fibrosis and stiffening of the tissue’s extracellular matrix, and a gradual decline in mesenchymal stromal cell function.
Metabolic conditions like type 2 diabetes and obesity accelerate many of these changes. Research has documented that adipose-derived cells from diabetic donors show reduced viability, altered secretome profiles, and decreased production of key growth factors. However, even diabetic adipose-derived cells retain significant functional capacity, including comparable immune-modulating properties to healthy donor cells.
Published research also suggests that adipose-derived mesenchymal stromal cells are more resilient to age-related decline than bone marrow-derived mesenchymal stromal cells, maintaining differentiation capacity through multiple culture passages and achieving over 50 population doublings.
This is the biological rationale behind banking tissue earlier rather than later, preserving the cellular ecosystem at a younger biological age. It is exactly that: a biological rationale based on published data about cellular aging, not a promise that younger tissue will produce better outcomes in any specific future application. The future clinical relevance of these differences remains to be determined by research that has not yet been completed.
Why Fat Health Matters for Future Regenerative Options
Connecting the dots carefully: adipose tissue provides one of the richest known sources of mesenchymal stromal cells, yielding approximately 500 times more cells per gram than bone marrow. These cells and their secretome are the subject of over 400 registered clinical trials on ClinicalTrials.gov spanning orthopedics, cardiovascular, neurological, autoimmune, and metabolic research areas.
The biological quality of harvested tissue at the time of banking may influence measurable laboratory outcomes such as cell yields, post-thaw viability, and proliferative capacity. Tissue collected from a healthier metabolic state, at a younger biological age, from the subcutaneous depot where mesenchymal stromal cell density is highest, may have different laboratory characteristics than tissue collected under less favorable conditions. Published data supports this at the level of lab measurements.
What the data does not support is a direct, guaranteed link between these laboratory measures and clinical benefit for any individual. The gap between “cells that look good in the lab” and “a therapy that helps a patient” is filled by clinical trials, regulatory review, product development, and evolving scientific evidence. None of that can be shortcut by the quality of the starting material alone.
Banking today preserves your adipose tissue and its full cellular ecosystem as it is right now, at your current biological age, through validated cryopreservation protocols. It creates an option for potential future use if and only if appropriate FDA-regulated opportunities arise, including clinical trials, Expanded Access programs, or future approved therapies that complete the full regulatory process.
What Banking Does and Does Not Do
What adipose tissue banking does:
It preserves your adipose tissue and its cellular ecosystem (including mesenchymal stromal cells, endothelial cells, immune cells, and the extracellular matrix) at your current biological age through validated cryopreservation protocols. Published research shows post-thaw viability rates of 80 to 91% using standard protocols, with preserved cell function documented after years of storage. Your tissue remains your property, stored under continuously monitored conditions.
What adipose tissue banking does not do:
It does not treat, cure, or prevent any disease. It does not enroll you in clinical trials or guarantee future access to any therapy or program. It does not guarantee that your banked tissue will ever be used clinically. It does not promise specific outcomes for you or your family. No adipose-derived mesenchymal stromal cell product or exosome product is FDA-approved to treat any condition in the United States as of March 2026. The only FDA-approved stem cell products are cord blood-derived hematopoietic progenitor cells for certain blood disorders.
Frequently Asked Questions
What does it mean that fat is an endocrine organ?
It means adipose tissue produces and secretes hormones and signaling molecules (adipokines) that travel through the bloodstream and influence distant organs, including the brain, pancreas, heart, and immune system. This was first established with the discovery of leptin in 1994 and has since been confirmed for dozens of additional signaling molecules.
Does losing weight damage my adipose-derived cells?
Weight loss reduces the size of fat cells (adipocytes shrink as they release stored energy) but does not destroy the mesenchymal stromal cells and other supporting cell populations within the tissue. The non-fat cell populations remain present in the tissue regardless of weight fluctuations. However, extreme or rapid weight changes can alter tissue biology in ways that are not fully characterized.
Do I need to be at my “perfect” weight to bank tissue?
No. Adipose tissue can be collected from adults across a wide range of body compositions. Published research has successfully isolated viable mesenchymal stromal cells from donors across a broad age and weight range. Banking does not require you to be at any specific weight. That said, the metabolic health of adipose tissue can vary depending on factors like visceral fat levels and inflammatory status.
If my adipose tissue is inflamed, does that mean banking is useless?
No. Even adipose tissue from donors with metabolic conditions retains functional cell populations. Published research has shown that cells from diabetic donors, for example, maintain significant immune-modulating properties. The tissue is preserved as it is at the time of collection, and the relevance of any inflammatory state to future clinical applications is not yet known.
Does banking adipose tissue improve my metabolic health now?
No. Banking is a preservation procedure, not a treatment. The mini-liposuction used to collect tissue removes a small volume (typically 100 to 200 mL) and has no meaningful impact on your overall metabolic health, body composition, or adipokine levels.
Are adipose-derived cells FDA-approved to treat any disease?
No. As of March 2026, no adipose-derived mesenchymal stromal cell product or exosome product is FDA-approved to treat any disease in the United States. The only FDA-approved stem cell products are cord blood-derived hematopoietic progenitor cells for certain blood disorders. Any future use of banked tissue must occur through legitimate FDA-regulated pathways.
What is the difference between subcutaneous and visceral fat for banking?
Subcutaneous fat (under the skin) is the primary source for adipose tissue banking because it has a higher concentration of mesenchymal stromal cells, a more favorable adipokine profile, and is easily accessible through minimally invasive liposuction. Visceral fat (around internal organs) has a more inflammatory cellular profile and is not typically harvested for banking.
Does the health of my fat at the time of banking matter for future use?
The biological state of your tissue at the time of collection may influence laboratory measures such as cell yield, viability, and proliferative capacity. Published data supports this at the level of lab measurements. However, there is no direct, proven link between these laboratory characteristics and specific clinical outcomes. The relevance of tissue quality to any future therapy will depend on the requirements of that specific product or protocol.
Can I do anything to improve the health of my adipose tissue before banking?
Maintaining a healthy metabolic state through balanced nutrition, regular physical activity, and management of conditions like diabetes or metabolic syndrome is generally associated with more favorable adipose tissue biology. However, Save My Fat does not provide medical advice, and any health decisions should be discussed with your own licensed healthcare provider.
How is this different from the stem cell treatments I see advertised?
Save My Fat provides a preservation service, not a treatment. Clinics marketing “stem cell treatments” for diseases are often offering products that have not been evaluated by the FDA for safety or effectiveness. The FDA has issued consumer alerts about unapproved regenerative medicine products. Tissue banking preserves your tissue for potential future use through legitimate, FDA-regulated pathways only.
Key Takeaways
Adipose tissue is an active endocrine organ that produces adipokines influencing appetite, insulin sensitivity, cardiovascular health, inflammation, and reproductive function. It is not passive storage.
Different fat depots behave differently. Subcutaneous fat (under the skin) has a more favorable metabolic and cellular profile than visceral fat (around organs), and is the primary source for tissue banking.
Adipose tissue contains a diverse cellular ecosystem beyond fat cells, including mesenchymal stromal cells, endothelial cells, pericytes, and immune cells, all of which contribute to the tissue’s biological activity and research interest.
Aging and metabolic disease alter adipose tissue biology through inflammation, senescent cell accumulation, and fat redistribution. This is the biological rationale for banking tissue earlier, though it is not a guarantee of better future outcomes.
Mesenchymal stromal cells from adipose tissue and their secretome are being studied in over 400 clinical trials, but no adipose-derived product is FDA-approved to treat any disease as of March 2026.
Banking preserves your adipose tissue and its cellular ecosystem at your current biological age through validated cryopreservation. It creates an option for potential future use within FDA-regulated pathways. It does not treat disease, guarantee access, or promise clinical benefit.
Ready to Learn More About Adipose Tissue Banking?
The biology of adipose tissue is more complex and more promising than most people realize. Understanding what your fat actually does, and what it contains, is the first step toward making an informed decision about whether tissue preservation aligns with your health planning goals.
Save My Fat helps individuals preserve adipose tissue through validated cryopreservation protocols for potential future use in FDA-regulated pathways. We focus on education, transparency, and realistic expectations.
Ready to learn more?
Visit: https://savemyfat.com Contact us: https://savemyfat.com/contact Learn about the process: How Stem Cell Banking Works
All medical decisions should be made in consultation with your own licensed healthcare professionals.
Save My Fat Adipose Tissue Banking for Future Regenerative Medicine Opportunities
Last updated March 10, 2026







